MRI tool to cure digestive disorders
Posted: 26 October 2018 | Drug Target Review | 3 comments
Purdue researchers have paved the way for more precise treatment for disorders in the gastrointestinal tract such as gastroparesis…
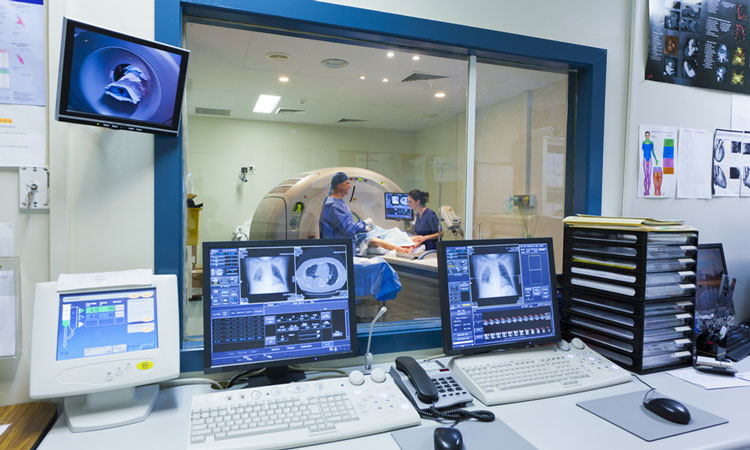
Huge numbers of people suffer from disorders in the gastrointestinal tract, with more than 60 million people in the US affected. The condition could be cured by electrical stimulation, but scientists don’t fully understand the therapy’s effects on a critical organ: the stomach.
Researchers at Purdue University used an MRI to show exactly how sending an electric impulse to the vagus nerve successfully corrects stomach complications. This technique could pave the way for more precise treatment that drugs and dietary changes have not been able to achieve.
“Eventually, by asking a patient to undergo multiple MRI scans with different electrical stimulation settings, we could figure out the best stimulation setting for alleviating that particular patient’s symptoms,” said Kun-Han “Tom” Lu, a PhD student in electrical and computer engineering. The research aligns with Purdue’s Giant Leaps celebration, acknowledging the university’s global advancements made in health, longevity and quality of life as part of Purdue’s 150th anniversary. This is one of the four themes of the yearlong celebration’s Ideas Festival, designed to showcase Purdue as an intellectual centre solving real-world issues.
The researchers mentioned how digestive disorders create a medical burden of billions of dollars every year. One important indicator of a digestive disorder is the rate at which the stomach empties of food, called “gastric emptying,” into the small intestine for the absorption of nutrients. Gastric emptying that is slow in pace in the disorder gastroparesis, means that stomach muscles aren’t moving properly.
The stimulation of this vagus nerve allows doctors to control how fast the stomach empties, effectively curing the condition.
“Some stimulation protocols for the stomach in humans already have FDA approval, but they’ve proved only partially effective,” said Dr Terry Powley, Purdue’s Distinguished Professor of Neuroscience and the director of the SPARC (Stimulating Peripheral Activity to Relieve Conditions) project, an initiative of the National Institutes of Health to map out the stomach’s neural circuitry. As part of the SPARC project, the researchers proposed using MRIs in small animals to get a better view of the effects of vagus nerve stimulation on the stomach.
“MRIs are non-invasive, show tissue contrast well and make it easier to repeat an experiment for verification,” Lu said.
Lu stimulated the vagus nerve to control the pyloric sphincter in rats, the valve that controls food leaving the stomach and entering the small intestine. He then created 3D reconstructions of MRI images over time. The images showed that stimulation relaxed the pyloric sphincter, speeding up gastric emptying to potentially correct delayed emptying in the case of gastroparesis, or other kinds of gastrointestinal malfunction.
“This method provides the physiological information for understanding the impacts of any treatment so that it can be fine-tuned for a specific organ or a specific disorder,” said Dr Zhongming Liu, Assistant Professor of Biomedical Engineering and Electrical and Computer Engineering.
The researchers plan to push the technology to retrieve even more information about gastric physiology and conduct their own tests of different treatments on gastric disorders.
The study was published as the cover of the journal Neurogastroenterology and Motility.
Related topics
Analysis, Analytical Techniques, Disease Research, Drug Discovery, Imaging, Research & Development, Screening, Therapeutics
Related conditions
gastrointestinal malfunction, gastroparesis
Related organisations
Purdue University
Related people
Dr Terry Powley, Dr Zhongming Liu, Kun-Han "Tom" Lu





Is there a possibility that furthering this research could lead to treating ACHALASIA? My daughter and thousands of others are diagnosed with this terrifying autoimmune disease. I search for medical advancements every day to find help.
Hi. What branch of the vagal stem do they stimulate for that particular valve in the stomach? Does the stimulated nerve move forward with progress is travel up and back the entire vagal stem? Are they able to stimulate the vagal stem higher up near a cranial nerve to aid in a malfunctioning esophagus (say Achalasia) with good results? Thanks.
There is a sub-set of gastroparesis (GP) patients whose symptoms began after stomach surgery. This is the “post-surgical” cohort, one of the least studied GP groups. This Purdue development in diagnosis makes me wonder if those of us who have post-surgical GP could benefit by determining the status of the vagus and the possible break site and having various kinds of stimulus aimed at the broken end of the vagus. Worth a try?
Another aspect of the GP story that is not discussed in the article above is that of bowel motility problems, which accompany stomach motililty troubles in most cases. Will the researchers also attempt to send ad monitor electrical stimulus to improve bowel motility? Here’s hoping they can do so!