First patient-derived organoid model for cervical cancer developed
Posted: 15 April 2021 | Victoria Rees (Drug Target Review) | No comments yet
Novel organoid models of cervical cancer and a healthy human cervix have been developed to study the condition and its progression.
A team of researchers led by the Hubrecht Institute, the Netherlands, have developed the first patient-derived organoid model for cervical cancer. They have also modelled the healthy human cervix using organoids.
The researchers used the organoid-based platform to study sexually transmitted infections for a herpes virus. They say that the model can potentially also be used to study the human papillomavirus (HPV), which is one of the main causes of cervical cancer.
According to the scientists, good models to study human cervical tissues are lacking, leading the researchers to develop their new organoid-based model for the healthy cervix and associated malignancies including cervical cancer.
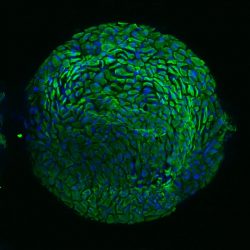
New cervical organoid model representing women’s protective armour [credit: Kadi Lõhmussaar, copyright Hubrecht Institute].
The researchers obtained human cervical tissue from either healthy patients or patients with different types of cervical cancer. The organoids were derived via a tiny bit of tissue obtained from patients’ Pap-brush material.
From these tissues the team grew organoids, tiny three-dimensional (3D) structures of about half a millimetre in size that closely mimic organ function. The organoids derived from healthy tissue closely resemble the tissue architecture and gene expression profiles of the actual human cervix. The organoids thus hold promise for studying what happens when a virus infects the human cervix.
Kadi Lõhmussaar, first author on the paper, explained: “For our study, we used a herpes virus – herpes simplex virus-1 (HSV-1) – to demonstrate the potential of the model for research into sexually transmitted infections… Cervical cancer is often caused by HPV-infection, but research into this virus was complicated as the virus is difficult to culture in the lab. Our new model might be able to overcome this obstacle.”
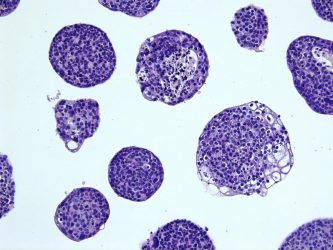
Histological view of a cancerous cervical organoid line [credit: Kadi Lõhmussaar, copyright Hubrecht Institute].
The researchers say the organoids grown from cancerous tissue – also called tumoroids – closely resemble actual tumours. They show mutation and gene expression profiles that are typical for cancer and carry similar morphological abnormalities. The team also found that the tumoroids respond differently to common chemotherapeutics, showing potential for precision medicine.
“Hopefully in the future, we can predict which chemotherapy will work best for specific patients based on results obtained in the tumoroids,” said Lõhmussaar.
The results were published in Cell Stem Cell.
Related topics
Disease Research, Oncology, Organoids, Precision Medicine
Related conditions
Cervical cancer, HPV
Related organisations
Hubrecht Institute
Related people
Kadi Lõhmussaar