Logic-gated DARPins show targeted T-cell activation in tumours
By Drug Target Review2025-12-08T09:00:32
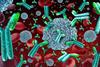
What if a T-cell therapy could activate only inside a tumour? New preclinical data on Molecular Partners’ Switch-DARPin suggest it may do just that.
Already a member? Sign in
Intelligence for the future of drug discovery
By highlighting cutting-edge research and its practical applications, Drug Target Review enables readers to make decisions that accelerate innovation, translate discoveries into therapies, and create tangible benefits for patients worldwide.
Become a member to continue reading
By becoming a member you join a connected and collaborative community driving the industry forward. Member benefits include:
- Unlimited access to industry intelligence that can make a difference to your business
- A weekly newsletter keeping the most vital information at the front of your thinking
- Exclusive invitations to powerful webinars and events featuring high profile experts
- Access to deep-dive reports and analysis that reveal exciting new opportunities for business growth and transformation
Related articles
-

-

-
 News
NewsHuman antimicrobial peptide dermcidin shows antiviral activity against influenza
2026-03-31T14:05:00Z
-
-

-

Partner content
-
 Whitepaper
WhitepaperWhitepaper: Targeting kinases in the innate immune response
2024-01-24T12:52:38
Sponsored by BellBrook Labs
-
 Whitepaper
WhitepaperApplication note: Solutions for your protein sample preparation workflow challenges
2023-11-20T13:43:43
Sponsored by Merck
-
 Whitepaper
WhitepaperApplication note: Direct and Competitive Live Cell Antibody Binding
2024-01-09T09:30:19
Sponsored by Sartorius
-
 Webinar
WebinarAI-powered drug discovery: Accelerating the development of life-saving therapies
2025-09-18T12:00:00
Sponsored by Benchling
-
 Webinar
WebinarThe future of carcinogenicity risk assessment: AI-powered, ethical alternatives to traditional testing
2025-04-02T14:00:00
Sponsored by Eurofins Discovery
-
 Whitepaper
WhitepapereBook: A Microscopy Guide For Spatial Biology
2023-12-11T10:49:07
Sponsored by Leica Microsystems
- Topics
- Technology
- Resources
- Diseases
- Drugs and therapies
- Research and development
- Tools and techniques
- Business
- Advertising & Editorial
- Advertising opportunities
- Media planner
- Advertising tech specs
- Information for authors
- Reuse policy
- Information
- About us
- Company information
- Careers
- Terms and conditions
- Privacy policy
- Cookie policy
- Topics A-Z
- Writers A-Z
- © 2026 Drug Target Review
Site powered by Webvision Cloud



