Psychedelic drugs such as psilocybin and MDMA may help repair the brain’s insulating myelin layer, according to new research.
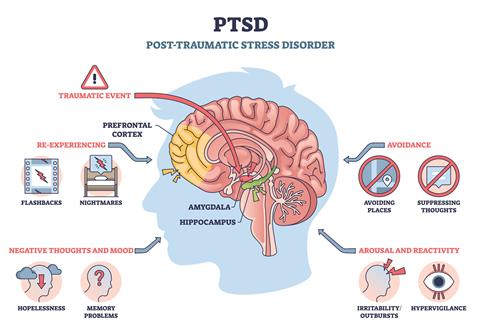
New research by Elsevier suggests that psychedelic drugs could help repair damage to the brain’s insulation system, potentially supporting longer-term recovery in people with post-traumatic stress disorder (PTSD).
The study indicates that treatment with psychedelics may trigger large-scale changes in brain network activity by remodelling myelin – the protective layer that insulates nerve cells.
Scientists say the findings point to a new biological mechanism that could help explain how psychedelic-assisted therapies deliver lasting benefits for conditions like PTSD.
From temporary effects to lasting change
Drugs including Psilocybin and 3,4-methylenedioxymethamphetamine (MDMA) are known to produce rapid clinical improvements in people with PTSD. However, researchers have been unsure how the brief psychedelic experience leads to more durable changes in brain function.
The new study suggests myelin may provide the missing link between the short-term effects of these drugs and longer-term stabilisation of neural circuits.
The new study suggests myelin may provide the missing link between the short-term effects of these drugs and longer-term stabilisation of neural circuits.
Scientists found that psychedelics stimulated activity-dependent oligodendrogenesis – the creation of specialised brain cells called oligodendrocytes that produce myelin. This process appeared to remodel the brain’s communication networks and restore healthier rhythms between circuits involved in threat detection and memory.
“The focus of psychedelic and MDMA research has been the effects of these drugs on neurons and neuroplasticity. This work has largely ignored a potentially important role for other cell types in the neurobiology of their therapeutic effects,” said John Krystal, MD, Editor of Biological Psychiatry. “Oligodendrocytes play a number of roles in the brain, which produce the myelin that insulates neurons. Subgroups of oligodendrocytes take up glutamate and contribute to glutamate homeostasis, protecting the brain from neurotoxicity. Another group of oligodendrocytes is involved in immune and inflammatory functions in the brain.”
Rat study reveals biological changes
To investigate further, researchers used a rat model of contextual fear conditioning. The animals were given repeated low doses of psilocybin or MDMA before undergoing behavioural testing.
Scientists monitored anxiety-like behaviour and exploration patterns while also analysing learning and memory performance.
The results showed a clear reduction in anxiety-like behaviour. This behavioural shift was accompanied by significant changes in oligodendrocyte biology and genetic activity linked to myelin remodelling in the dentate gyrus – a region within the hippocampus that plays a central role in memory.
“To test whether myelin integrity was simply associated with behavioural change – or actually required for it – we combined the drug interventions with models that either damaged brain insulation (demyelination) or chemically enhanced it (promyelination) to see how these changes affected recovery,” said lead investigator of the study Dr Mehmet Bostancıklıoğlu from the Department of Physiology at Gaziantep University Faculty of Medicine.
 A novel study in Biological Psychiatry identifies myelin plasticity after treatment with psychedelics as the missing link towards long-term PTSD recovery, triggering a large-scale reconfiguration of brain network dynamics. Credit: Biological Psychiatry / Bostancıklıoğlu et al.[/caption]
A novel study in Biological Psychiatry identifies myelin plasticity after treatment with psychedelics as the missing link towards long-term PTSD recovery, triggering a large-scale reconfiguration of brain network dynamics. Credit: Biological Psychiatry / Bostancıklıoğlu et al.[/caption] Evidence of physical repair
Using advanced microscopy and genetic analysis the team confirmed that both psilocybin and MDMA stimulated physical repair of myelin.
Using advanced microscopy and genetic analysis the team confirmed that both psilocybin and MDMA stimulated physical repair of myelin.
When scientists blocked a key serotonin receptor known as 5-HT2A both the behavioural improvements and the myelin changes disappeared. However, when researchers used anisomycin to block the formation of fear memories, anxiety levels still dropped but myelin damage remained.
This suggests that suppressing traumatic memories alone may not be enough for full biological recovery.
“Overall, this data suggest that psychedelics and MDMA, like selective serotonin reuptake inhibitors (SSRIs) and ketamine, may promote the recovery from stress-related damage to myelin, contributing to clinical recovery,” said Dr Krystal.
Supporting psychotherapy rather than replacing it
The researchers also observed that psilocybin and MDMA reduced astrocyte reactivity, which is usually connected to brain inflammation.
However, the authors emphasise that boosting myelin repair would not replace psychological therapy. Instead they suggest it may help consolidate the positive neural changes that occur after a psychedelic treatment session.
“We often talk about psychedelics as ‘opening a window’ for brain plasticity. Recent work emphasises that these drugs can acutely loosen entrenched network patterns and then leave a sub-acute period in which experience can reshape circuits,” said Dr Bostancıklıoğlu. “What we show here is that myelin-producing cells may be an underappreciated part of that story – helping translate a transient window into longer-lasting circuit change, at least in a fear-based rat model.”