Scientists at the Medical University of Vienna identify multiple mechanisms of multidrug resistance in Candida auris, revealing new therapeutic opportunities.
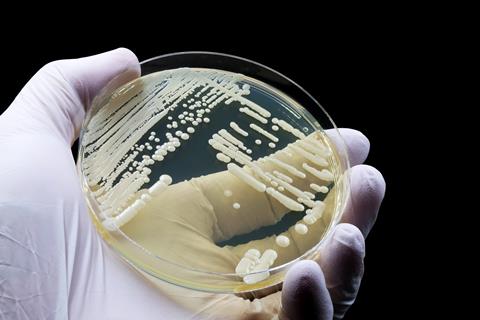
The emerging fungal pathogen Candida auris represents one of the most urgent threats worldwide. Since its first identification in 2009, C. auris has spread rapidly across all six continents and is now reported in more than 60 countries. Its exceptional ability to persist on human skin, transmit efficiently in healthcare settings and tolerate multiple antifungal drug classes has led the World Health Organization to classify C. auris as a priority fungal pathogen requiring urgent research and therapeutic innovation.1
Despite intense global effort, treatment options for C. auris infections remain limited, with the pathogen showing resistance to multiple antifungal drugs, including Azoles, amphotericin B and, while less common, echinocandin resistance remains a clinical concern. Understanding the molecular basis of this intrinsic and acquired drug tolerance is therefore critical for identifying new therapeutic vulnerabilities.
A recent study2 by researchers at the Vienna Biocenter, Medical University of Vienna applied an integrated proteo-transcriptomic approach to uncover previously unrecognised metabolic strategies underpinning both skin colonisation and antifungal drug tolerance in Candida auris. The findings reveal a central role for carbon dioxide (CO2) sensing and mitochondrial metabolism, opening new avenues for antifungal drug targeting.
Skin colonisation and hospital transmission
Unlike other pathogenic Candida species, C. auris displays a pronounced tropism for human skin. The organism adheres efficiently to the epidermis, survives desiccation and persists on medical equipment and hospital surfaces. For immunocompromised patients, skin colonisation frequently precedes invasive infection and is associated with mortality rates approaching 70 percent in some cohorts.1
The skin is a challenging ecological niche, characterised by low pH, osmotic pressure and low nutrient availability. How C. auris adapts to these conditions while maintaining robust growth and high antifungal tolerance has remained largely unexplained.
A comprehensive proteo-transcriptomic strategy
To address this question, the authors combined quantitative proteomics with transcriptomic profiling for drug resistance and sensitive clinical strains. This integrated approach enabled the identification of coordinated regulatory programmes that are not apparent from transcriptomics alone.
We observed extensive redundancy and complementarity in drug resistance mechanisms in Candida auris. Its pronounced resistance to the commonly used drug fluconazole does not rely on a single change, but instead arises from multiple concurrent strategies.
The dataset revealed extensive remodelling of membrane transport systems, with more than 30 transporters among the 92 differentially regulated proteins in a multidrug-resistant strain.2 These included well-characterised multidrug efflux pumps such as Cdr1 and Mdr1,3 as well as the phosphatidylinositol transfer protein Pdr16.4
First author Trinh Phan-Canh said: “We observed extensive redundancy and complementarity in drug resistance mechanisms in Candida auris. Its pronounced resistance to the commonly used drug fluconazole does not rely on a single change, but instead arises from multiple concurrent strategies, including mutations in lanosterol 14α-demethylase and the regulated expression of several membrane transporters. Together, these mechanisms form a coordinated network that determines the level of resistance in specific clinical strains.”
Beyond transporters, proteomic profiling surprisingly highlighted a strong enrichment of proteins involved in CO2 sensing, mitochondrial respiration and carboxylic acid metabolism. These pathways emerged as core determinants of both drug tolerance and skin fitness.
CO2 sensing links metabolism to drug resistance
A key study finding was the identification of a CO2-dependent metabolic adaptation that enables C. auris to thrive under nutrient-limited skin conditions. Central to this process is carbonic anhydrase, an enzyme that catalyses the reversible conversion of CO2 into bicarbonate.
In ambient air, carbonic anhydrase allows C. auris to fix a small amount of CO2, which sustains its energy metabolism. This metabolic pathway compensates for nutrient scarcity and mitigates the cellular stress imposed by antifungal drugs, particularly amphotericin B.
Genetic disruption confirmed that impairment of this CO2-sensing pathway significantly reduces fungal fitness on skin-mimicking substrates and resensitises this fungus to antifungal treatment. These findings establish CO2 metabolism as a previously unrecognised driver of amphotericin B resistance in C. auris.

Illustration showing how the carbonic sensing pathway controls fitness and amphotericin B resistance in
Candida auris. Credit: Vienna BioCenter / Trinh Phan-Canh[/caption]
More importantly, the study showed that several clinical Candida auris isolates acquire increased tolerance to amphotericin B under elevated CO2 conditions. This finding suggests that amphotericin B may be less effective once the fungus enters the bloodstream, where CO2 levels are substantially higher than on the skin surface.
Interactions with ESKAPE bacteria
Recent clinical observations have consistently reported co-colonisation of Candida auris with ESKAPE bacteria, particularly Klebsiella pneumoniae.5,6 The present study provides a mechanistic explanation for this phenomenon. Specifically, C. auris can exploit CO2 produced by urease-positive bacteria, including Klebsiella pneumoniae and Proteus mirabilis, which are frequently implicated in nosocomial transmission and spread via skin contact in hospital environments. These bacteria degrade urea – present at high levels in human sweat – resulting in local CO2 release. This bacterially derived CO2 serves as an additional metabolic resource for C. auris, supporting mitochondrial energy metabolism and persistence under nutrient-limited conditions. While this study directly demonstrates the interaction with urease-positive nosocomial bacteria, it is plausible that other skin-associated microbes with similar metabolic activity could contribute in a comparable manner.
What a fascinating example of microbial communication. When Trinh first brought this to me, I was absolutely amazed.
From an infection-control perspective, these findings suggest that disrupting bacterial urease activity or limiting local CO2 availability may represent an indirect strategy to reduce C. auris skin colonisation and transmission in healthcare environments.
Prof Karl Kuchler commented: “What a fascinating example of microbial communication. When Trinh first brought this to me, I was absolutely amazed. This phenomenon makes a great deal of sense in the context of interkingdom interactions between Candida auris and other skin microbes. Urea is present on human skin through sweat and is also widely used in skincare products. This helps explain why C. auris thrives in this niche, particularly when it co-colonises with other bacteria, as we observe in clinical settings.”
Rethinking amphotericin B resistance
For more than a decade, amphotericin B resistance in C. auris has been primarily attributed to alterations in ergosterol biosynthesis. While such mutations do occur, they are relatively rare in clinical isolates and fail to fully explain the consistently high tolerance of this species compared with other Candida pathogens such as C. albicans or C. glabrata.3
The current study provides a mechanistic explanation for this long-standing paradox. CO2-dependent metabolic adaptation and mitochondrial respiration promote amphotericin B tolerance independently of ergosterol composition. This challenges the prevailing paradigm that sterol alteration is the dominant determinant of amphotericin B susceptibility and highlights metabolism-driven resistance mechanisms as critical.
Mitochondrial cytochrome bc1 as a drug target
Among the most therapeutically relevant findings is the identification of mitochondrial cytochrome bc1 as a key vulnerability within the CO2-dependent metabolic network. Pharmacological inhibition of cytochrome bc1 markedly impaired fungal energy metabolism and restored amphotericin B efficacy in experimental models.
The study reports a lead compound with specificity for fungal cytochrome bc1, providing proof-of-concept that metabolic co-targeting can potentiate existing antifungals. While further optimisation and safety profiling are required, this approach exemplifies how metabolic pathway inhibition can be leveraged to overcome intrinsic drug tolerance.
Prof Adelheid Elbe-Bürger added: “Inhibiting cytochrome bc1 can suppress the growth of Candida auris and enhance killing by amphotericin B. Although the fungal-specific inhibitor Inz-5 [that] we used showed promising activity, further structure–activity relationship studies are needed to improve its in vivo stability. Nevertheless, our findings indicate that cytochrome bc1 represents a promising antifungal drug target, particularly in combination with amphotericin B.”
Implications for antifungal drug development
The number of severe Candida auris infections has been rising worldwide for more than 15 years, while the underlying mechanisms are still poorly understood. These new findings decipher key survival strategies of the pathogen and provide an important basis for the development of urgently needed therapeutic approaches.
References
- Chowdhary A, Lionakis MS, Chauhan N. Candida auris: host interactions, antifungal drug resistance, and diagnostics. Microbiol. Mol. Biol. Rev. e00187-22 (2025).
- Phan-Canh T, et al. Candida auris skin tropism and antifungal resistance are mediated by carbonic anhydrase Nce103. Nat. Microbiol. 11, 461–475 (2026). https://doi.org/10.1038/s41564-025-02189-z
- Rybak JM, Cuomo CA, Rogers DP. The molecular and genetic basis of antifungal resistance in the emerging fungal pathogen Candida auris. Curr. Opin. Microbiol. 70, 102208 (2022).
- Phan-Canh Trinh, Bitencourt T, Kuchler K. Gene dosage of PDR16 modulates azole susceptibility in Candida auris. Microbiol. Spectr. 0, e02659-24 (2025).
- Proctor DM, et al. Integrated genomic, epidemiologic investigation of Candida auris skin colonization in a skilled nursing facility. Nat. Med. 27, 1401–1409 (2021).
- Proctor DM, et al. Clonal Candida auris and ESKAPE pathogens on the skin of residents of nursing homes. Nature 639, 1016–1023 (2025).
Meet the experts
 Dr Trinh Phan-Canh
Dr Trinh Phan-Canh
Dr Phan-Canh is a molecular microbiologist based at the Vienna BioCenter with a strong background in medical mycology and fungal pathogenesis. His work combines multiomics technologies with targeted genetic and phenotypic approaches to elucidate mechanisms of antifungal resistance and host–fungal interactions, with a particular focus on Candida auris. His study on skin adaptation and drug resistance in C. auris was highlighted on the cover of the February 2026 issue of Nature Microbiology.
 Prof Karl Kuchler
Prof Karl Kuchler
Prof Kuchler is a molecular biologist whose research centres on host–pathogen dynamics and fungal infections. At the Medical University of Vienna and the Max Perutz Labs Vienna, he established innovative systems biology and functional genomics strategies to investigate transcriptional regulation, virulence traits, antifungal resistance and immune recognition in fungal pathogens. Across more than 30 years, he has played a significant role in advancing the field of infection biology.
 Prof Adelheid Elbe-Bürger
Prof Adelheid Elbe-Bürger
Prof Elbe-Bürger heads the “Cellular and Molecular Immunobiology of the Skin” group at the Medical University of Vienna. Her research addresses immune system development and function in human skin across different life stages. Through human ex vivo skin models, her team explores mechanisms of cutaneous inflammation, tissue repair and antimicrobial intervention strategies.




















