Researchers are targeting epithelial dysfunction by using repurposed cancer therapeutics to address the underlying pathology driving Crohn’s Disease.
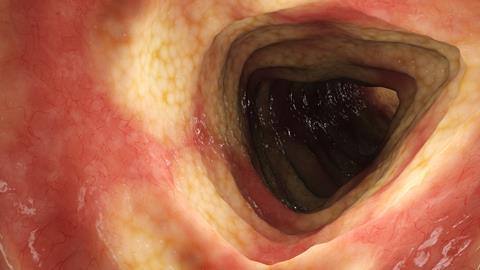
Biologists at the University of Houston have contributed to a potential breakthrough in the treatment of Crohn’s disease by moving their focus from managing symptoms to addressing a key underlying cause of the condition.
Roughly 6 to 10 million people worldwide are estimated to be living with Crohn’s disease or ulcerative colitis, with Crohn’s characterised by a damaging cycle in which the immune system attacks the epithelial lining of the gut, weakening the gut barrier. When this protective lining fails to repair itself, bacteria and toxins can leak into the body, driving ongoing inflammation and worsening the disease.
Roughly 6 to 10 million people worldwide are estimated to be living with Crohn’s disease or ulcertative colitis
Current treatments rely largely on anti-inflammatory drugs to control flare-ups. However, these therapies are only partially effective, with just around 20 percent of patients achieving long-term remission.
The researchers behind this new study suggest that the disease is driven by defects in the epithelial lining itself, which in turn trigger the immune response. By repurposing two existing cancer drugs, they aim to halt this cycle and allow the gut to heal.
“It’s a paradigm shift from the way we’ve thought about the disease,” said Seema Khurana, Senior Author and Moores Professor of Biology and Biochemistry at the University of Houston. “Existing therapies primarily manage symptoms because we don’t know what causes the disease. We believe our research brings us closer to identifying those drivers.”
Targeting the stress signal
Khurana has been researching gastroenterology for nearly three decades and previously explored the role of the gut barrier in Crohn’s disease. Her team’s earlier work identified how chronic stress within the intestines can lead to the destruction of epithelial cells rather than their regeneration.
The latest findings build on this by showing that dysfunction in these cells not only damages the gut lining but also actively prevents it from repairing.
“In a healthy cell the stress signal goes up and when the stress is resolved, the signal goes back down. In Crohn’s patients, this stress signal is always on,” Khurana said. “When the stress signal is always on the cell cannot manage the stress and undergoes a form of programmed cell death called necroptosis, which further triggers inflammation.”
The researchers found that low doses of two cancer drugs, Pazopanib and Ponatinib, could interrupt this harmful process. Both medications appear to block the stress signals and prevent cell death, allowing the intestinal lining to repair itself naturally.
Faster route to patient care
Repurposing existing drugs offers many advantages in bringing treatments to patients more quickly. Because these medications have already been approved by the US Food and Drug Administration, the risks and costs associated with developing entirely new drugs are greatly reduced.
Repurposing existing drugs offers many advantages in bringing treatments to patients more quickly
“If you had to start from scratch to identify and develop a drug, it takes 10 to 15 years and can cost between $1 billion to $2 billion,” Khurana said. “For a patient who is suffering from chronic Crohn’s disease, they’re looking for some immediate relief. Our goal was to make our findings much more translatable to real patients.”
The researchers believe their approach could lead to new effective treatments that address the root causes of Crohn’s disease, potentially improving outcomes for patients who do not respond to existing therapies.














No comments yet