Japanese researchers have shown in a rat study that stem cells derived from naturally shed baby teeth may improve motor and cognitive impairments in chronic-phase cerebral palsy.
A research team from Nagoya University Hospital has reported promising findings that could lead to new treatments for cerebral palsy, even after symptoms have already developed.
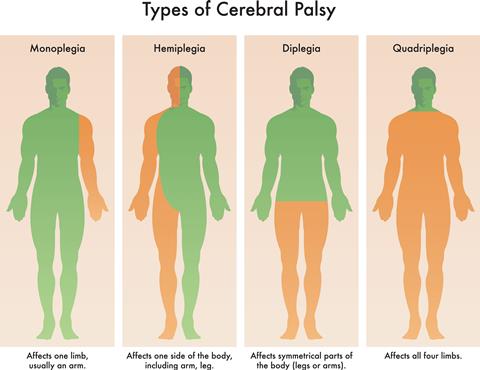
Understanding cerebral palsy
Cerebral palsy is a neurological condition most commonly caused by brain damage before or during birth, leading to impaired posture and movement. Early signs are often subtle and diagnosis may be delayed until more obvious symptoms occur as a child grows.
The condition affects two to three in every 1,000 live births and there is currently no cure. The primary cause is hypoxic-ischemic encephalopathy, a form of brain injury resulting from reduced oxygen and blood flow.
In recent years, animal studies have suggested that stem cell therapy may help restore neurological function if administered in the acute or subacute phase, typically within a few weeks after birth.
In recent years, animal studies have suggested that stem cell therapy may help restore neurological function if administered in the acute or subacute phase, typically within a few weeks after birth. Some clinical research has indicated possible benefits even at later stages, although confirmatory clinical trials have yet to be published.
Now, researchers have demonstrated in rat experiments that stem cells derived from human primary tooth pulp may offer therapeutic benefit in the chronic phase of cerebral palsy.
“This is the first animal study to show that stem cell treatment works even after motor deficits have already appeared,” said Clinical Professor Yoshiaki Sato of Nagoya University Hospital and the study’s corresponding author.
 Mechanism of SHED-derived HGF in treating chronic perinatal brain injury. Credit: Yoshiaki Sato.[/caption]
Mechanism of SHED-derived HGF in treating chronic perinatal brain injury. Credit: Yoshiaki Sato.[/caption] Animal model experiments
To replicate the condition, researchers induced unilateral hypoxic-ischemic brain injury in seven-day-old rats, producing one-sided motor impairment similar to hemiplegic cerebral palsy in humans. At four weeks of age, the animals were assessed using a horizontal ladder test, with only those demonstrating significantly impaired performance included in the study.
In the horizontal ladder test, which required rats to cross irregularly spaced rungs, those given SHED recorded significantly fewer slips than controls at four months.
The selected rats received intravenous stem cells from human exfoliated deciduous teeth (SHED) during the chronic phase at five, seven and nine weeks of age, roughly corresponding to pre-adolescence in humans.
Motor and learning functions were compared between treated and untreated groups. In the horizontal ladder test, which required rats to cross irregularly spaced rungs, those given SHED recorded significantly fewer slips than controls at four months.
In the cylinder test, designed to measure forelimb asymmetry, treated rats relied more on their impaired forelimb. In the shuttle avoidance test, they achieved significantly higher avoidance rates in later sessions, indicating improved learning and memory.
Using quantum dot-labelled SHED and in vivo imaging, the team confirmed that the transplanted cells migrated to the brain.
Cell culture findings and next steps
Further laboratory experiments compared SHED with other stem cell types, including bone marrow mesenchymal stromal cells and dermal fibroblasts. In non-contact co-culture conditions, SHED promoted neural stem cell proliferation more effectively than the alternatives, an effect attributed to their high secretion of hepatocyte growth factor.
The researchers concluded that SHED therapy may improve both motor and cognitive impairments in chronic-phase cerebral palsy models by stimulating new nervous tissue growth.
Nagoya University Hospital is now conducting a clinical study to evaluate the safety and tolerability of a single intravenous dose of autologous SHED in children with cerebral palsy. Depending on the results, the team intends to pursue larger trials and long-term follow-up.
“Our ultimate goal is to establish this approach as a new treatment option for patients with cerebral palsy and their families,” Sato said.




















