Osaka Metropolitan University researchers have identified two antimicrobial treatments that may effectively combat severe hemorrhagic pneumonia caused by multidrug-resistant Stenotrophomonas maltophilia.
Researchers at Osaka Metropolitan University have found that two antimicrobial treatments may help to fight against severe cases of hemorrhagic pneumonia caused by the multidrug-resistant bacterium Stenotrophomonas maltophilia which poses a growing threat to immunocompromised patients.
The bacterium, commonly referred to as S. maltophilia, can trigger life-threatening lung infections in people with weakened immune systems. However, treatment options remain limited and infections are difficult to manage due to rising antimicrobial resistance.
Study compares two treatments
The study was led by Dr Waki Imoto at the university’s Graduate School of Medicine investigated the effectiveness of two antibiotics, levofloxacin (LVFX) and cefiderocol (CFDC), in a mouse model designed to replicate severe hemorrhagic pneumonia caused by S. maltophilia.
Levofloxacin is seen as one of the most effective treatments available for the infection. Yet reports of bacterial resistance to the drug have increased in recent years, raising concerns among clinicians about its long-term reliability.
Cefiderocol, a newer antimicrobial agent, has shown promising activity against S. maltophilia in previous experimental studies. Until now, however, its effectiveness against hemorrhagic pneumonia caused by the bacterium had not been fully understood.
To assess the two treatments, researchers separated mice into three groups: a control group, a cefiderocol treatment group and a levofloxacin treatment group. The animals were then given severe hemorrhagic pneumonia caused by S. maltophilia before receiving the respective therapies.
Improved survival and reduced lung damage
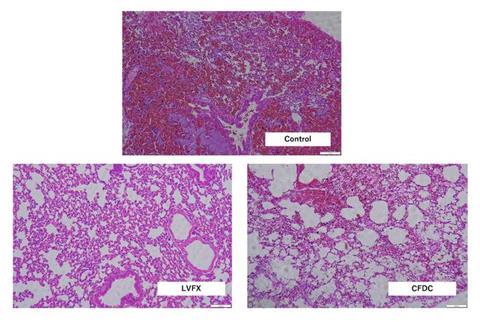
The study saw that both antimicrobial treatments improved survival rates among the mice and reduced bacterial levels in the lungs and heart.
Researchers also observed signs of reduced lung damage in both treatment groups. Microscopic examination of lung tissue revealed lower levels of haemorrhaging, suggesting the drugs helped suppress the destructive effects of the infection.
Despite these positive findings, the researchers noted differences in outcomes between the two therapies.
Mice treated with levofloxacin rarely showed signs of haemorrhage, while those treated with cefiderocol experienced slight occurrences of bleeding in lung tissue.
“The effects observed in this study were more pronounced with LVFX. One possible reason is that it more readily reaches the lungs, which are the primary organs infected by the bacteria,” said Dr Imoto.
Concerns over antibiotic resistance
Although levofloxacin appeared to produce stronger results in the study, researchers warned that increasing antimicrobial resistance could limit its future effectiveness.
“On the other hand, because the emergence of LVFX-resistant strains has been reported, it is important to select appropriate therapeutic agents depending on the clinical situation while taking antimicrobial resistance into account and using CFDC as an alternative treatment for S. maltophilia,” Dr Imoto added.
Researchers believe cefiderocol could become an important back-up treatment option for difficult S. maltophilia infections, particularly in cases where resistance to conventional antibiotics is detected.















No comments yet