Using a straightforward cell stacking method, researchers have regenerated functional lymph nodes, offering a potential long-lasting therapy for secondary lymphedema and creating new opportunities for immunology and oncology drug discovery.
The global rise of cancer has led to a growing number of surgical procedures involving the removal of lymph nodes. While these operations are essential for cancer staging and limiting the spread of disease, they can leave patients with serious long-term complications. One of the most debilitating is secondary lymphedema, a condition caused by the permanent loss of lymph nodes, which do not regenerate naturally once removed.
Secondary lymphedema’s symptoms include chronic swelling, pain and reduced mobility in affected limbs or body regions. These symptoms can occur for life, placing a long-term burden on healthcare systems.
Now, a new study from researchers at the Tokyo University of Science presents an alternative, a simple and reproducible method to bioengineer lymphatic tissue capable of restoring lymphatic flow after lymph node removal.
A centrifugal approach to tissue engineering
Regenerative medicine has increasingly sought ways to restore damaged lymphatic structures. To date, most approaches have focused on stem cell therapies or lymphatic tissue transplantation. However, these strategies often require complex preparation and have shown limited success in improving the key clinical symptoms of lymphedema.
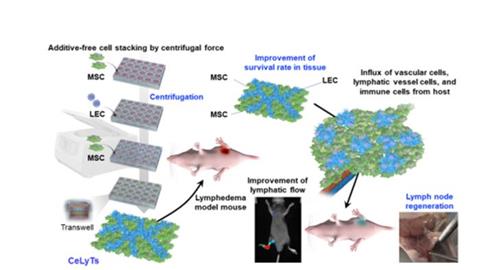
In an effort to overcome these difficulties, the Tokyo researchers developed a centrifugal cell stacking technique to produce centrifuge-based bioengineered lymphatic tissue (CeLyT). Mesenchymal stem cells were first centrifuged to form a uniform base layer, followed by lymphatic endothelial cells to create a second layer and a final mesenchymal stem cell layer. This three-layered structure was designed to replicate the architecture and function of native lymph nodes.
Restoring lymphatic and immune function
When tested in a mouse model of lymphedema, CeLyTs successfully restored lymphatic flow following removal of the popliteal and inguinal lymph nodes. Swelling in the paws and legs improved markedly, returning to near-normal levels within weeks.
When tested in a mouse model of lymphedema, CeLyTs successfully restored lymphatic flow following removal of the popliteal and inguinal lymph nodes.
The transplanted mice also demonstrated recovery of lymph node functions, including filtration capacity and immune cell populations such as T cells and macrophages. Fat accumulation in affected tissues was reduced to levels comparable with healthy animals.
“CeLyTs may initially induce lymph and blood vessel formation around the transplantation site, leading to the establishment of an immature lymph node-like structure formed by incorporating host-derived cells into the tissue within several days, followed by its maturation and ability to function as a lymph node within 10 days after transplantation,” said Kosuke Kusamori, Associate Professor at the Faculty of Pharmaceutical Sciences at Tokyo University of Science.
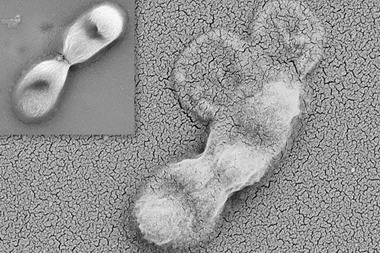
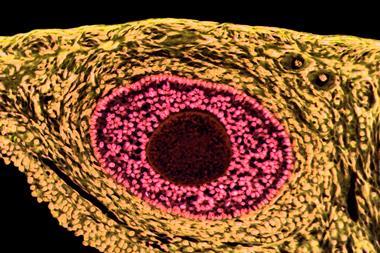
 Researchers engineer centrifuge-based lymphatic tissue for the treatment of secondary lymphedema that occurs after lymphadenectomy. Credit: Associate Professor Kosuke Kusamori from Tokyo University of Science, Japan.[/caption]
Researchers engineer centrifuge-based lymphatic tissue for the treatment of secondary lymphedema that occurs after lymphadenectomy. Credit: Associate Professor Kosuke Kusamori from Tokyo University of Science, Japan.[/caption] Implications for drug discovery and development
Beyond its therapeutic potential, the study has significant relevance for drug discovery. The ability to regenerate functional lymph nodes provides new insight into lymphangiogenesis, immune cell trafficking and lymph node maturation, all of which are key biological processes targeted in oncology and immunology drug development.
Beyond its therapeutic potential, the study has significant relevance for drug discovery.
Bioengineered lymphatic tissues such as CeLyTs could also function as advanced experimental models for testing drugs that influence immune responses, inflammation and lymphatic function, offering more physiologically relevant alternatives to conventional cell cultures.
A shift in lymphedema treatment
This is the first reported regeneration of fully functional lymph nodes through cell transplantation. A single transplantation could provide durable benefits, reducing the need for lifelong compression therapy and repeated clinical care.
“Although compression therapy represents the gold standard for the treatment of lymphedema in clinical practice, it usually delays the swelling in the paws of lymphedema mice,” says Dr Kusamori. “By contrast, CeLyTs were more effective at suppressing lymphedema, also exhibiting strong therapeutic effects even in a more severe chronic lymphedema model. Moreover, CeLyTs demonstrated a greater lymphedema-suppressive effect, compared with bioengineered tissues fabricated by other tissue engineering methods.”
Topics
- 3D Cell Cultures
- Biotechnology & Bioengineering
- Cancer
- Cancer
- Cell & Gene Therapy
- Disease Research
- Drug Development
- Drug Discovery Processes
- Ex Vivo Models
- Immunology
- Immuno-oncology
- Immunotherapy
- In Vivo Testing
- Kosuke Kusamori (Associate Professor at the Faculty of Pharmaceutical Sciences at Tokyo University of Science)
- lymphedema
- Molecular Biology
- Neurological disorders
- Oncology
- Regenerative Medicine
- Regenerative Medicine
- Regenerative Medicine dupe
- Stem Cells
- Technology
- the Tokyo University of Science
- Translational Science