Scientists have discovered that specialised immune cells in the eye help keep its drainage system clear and regulate pressure, which could inform new treatments for glaucoma.
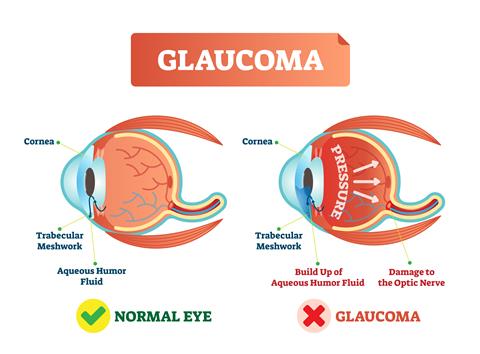
New research from Duke University has discovered a previously unknown role for immune cells in regulating pressure inside the eye.
The study shows that specialised immune cells act as a kind of microscopic cleaning crew in the eye’s drainage system. By keeping this system clear, the cells help maintain healthy eye pressure and prevent the damage that can lead to vision loss.
The discovery could also provide a new therapeutic target for future treatments aimed at tackling the underlying causes of glaucoma rather than simply managing its symptoms.
How eye pressure leads to damage
Inside the eye, fluid continuously drains through a delicate system of channels. When this drainage pathway becomes blocked, pressure can build up. Over time, the increased pressure can damage the optic nerve and lead to glaucoma.
Inside the eye, fluid continuously drains through a delicate system of channels.
Current treatments focus on lowering eye pressure, usually through medication or surgery. However, these approaches do not always prevent progressive vision loss.
“The only way we can treat glaucoma is by lowering the eye pressure, yet we still have patients who go blind despite current treatments,” said Dr Katy Liu, MD, lead author of the study and Assistant Professor in the Department of Ophthalmology at the Duke University School of Medicine. “This research helps us understand the role of the immune system in regulating eye pressure.”
The eye’s microscopic ‘clean up crew’
The study focused on immune cells known as resident macrophages. These cells live within the tissues that form the eye’s drainage system but until now scientists did not know whether they played a role in controlling pressure.
Using fluorescent markers, researchers tracked these cells in the eyes of mice. The team then selectively removed the macrophages to observe what would happen.
Without them, the drainage pathway quickly became clogged. Fluid accumulated and pressure inside the eye rose significantly.
“Our findings show that resident macrophages are essential for maintaining healthy eye pressure,” said Liu. “Disruption of this system may contribute directly to the development of glaucoma.”
A new direction for glaucoma treatment
The discovery suggests that therapies designed to support or restore these immune cells could help maintain proper fluid drainage in the eye.
The discovery suggests that therapies designed to support or restore these immune cells could help maintain proper fluid drainage in the eye.
According to the researchers, the next step will be identifying and studying these resident macrophages in human eye tissue to confirm that the same mechanism operates in people.
“Now we have a specific target for developing new therapies that can normalise the eye pressure and stop vision loss, in contrast to current medications that do not target the source of disease,” said Dr William Daniel Stamer, corresponding author, Joseph A.C. Wadsworth Distinguished Professor of Ophthalmology and Co-vice Chair for Basic Science Research.
Building on a history of breakthroughs
These findings add to a long track record of glaucoma research at the Duke Eye Center, including work that helped lead to approval by the US Food and Drug Administration of the first new glaucoma drug in two decades.
“This discovery is a major step forward in understanding how the immune system contributes to the regulation of eye pressure,” said Dr Daniel Saban, co-corresponding author, Joseph A.C. Wadsworth Distinguished Professor of Ophthalmology and Vice Chair of Research Strategy in the Department of Ophthalmology. “This research builds on Duke's strong history of turning laboratory findings into real treatments for patients.”
Researchers hope that further work could eventually lead to treatments capable of preventing glaucoma before irreversible damage occurs.
Topics
- Analytical Techniques
- Artificial Intelligence (AI)
- Biologics
- Biomarkers
- Biopharmaceuticals
- Biotherapeutics
- Cancer
- Companies
- Computational Techniques
- Drug Development
- Drug Discovery
- Drug Discovery Processes
- Drug Targets
- Duke University
- Machine Learning (ML)
- Molecular Biology
- Molecular Targets
- Monoclonal Antibodies
- Proteomics
- Translational Science