Researchers have shown that using CRISPR to disable the NRF2 gene can restore chemotherapy sensitivity and slow tumour growth.
Scientists at ChristianaCare’s Gene Editing Institute have reported a new discovery in cancer treatment after demonstrating that disabling a key gene using CRISPR technology can restore chemotherapy sensitivity in lung cancer. Their findings, show that targeting the NRF2 gene reverses drug resistance and slows tumour growth in both laboratory and animal studies.
The work represents more than a decade of research into NRF2, a gene known to drive treatment resistance across several cancer types. According to the team, the consistency of results across multiple models forms a basis for future clinical testing.
“We’ve seen compelling evidence at every stage of research,” said Dr Kelly Banas, lead author of the study and Associate Director of Research at the Gene Editing Institute. “It’s a strong foundation for taking the next step toward clinical trials.”
Potential beyond lung cancer
The study centres on lung squamous cell carcinoma, an aggressive form of non-small cell lung cancer (NSCLC) that makes up for around 30 percent of all lung cancer diagnoses. The American Cancer Society estimates that more than 190,000 people in the United States will be diagnosed with lung cancer in 2025.
This is a significant step toward overcoming one of the biggest challenges in cancer therapy – drug resistance.
Although the research focused on this subtype, the implications reach much further afield. Overactive NRF2 has long been linked to chemotherapy resistance in several solid tumours, including liver, oesophageal and head and neck cancers. By applying CRISPR to disrupt NRF2, researchers believe a similar strategy could help resensitise multiple tumour types to standard drug regimens.
“This is a significant step toward overcoming one of the biggest challenges in cancer therapy – drug resistance,” Banas said. “By targeting a key transcription factor that drives resistance, we’ve shown that gene editing can re-sensitise tumours to standard treatment. We’re hopeful that in clinical trials and beyond, this is what will allow chemotherapy to improve outcomes for patients and could enable them to remain healthier during the entirety of their treatment regimen.”
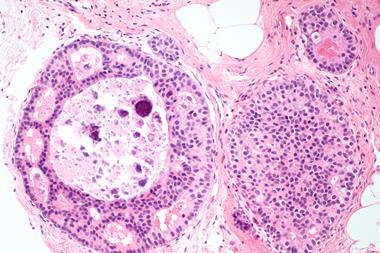
 Digitally modified image of tumour cells with CRISPR/Cas9 affected cells in brown. Credit: Gene Editing Institute[/caption]
Digitally modified image of tumour cells with CRISPR/Cas9 affected cells in brown. Credit: Gene Editing Institute[/caption] Targeting a master switch for resistance
Scientists honed in on a tumour-specific mutation known as R34G in the NRF2 gene. NRF2 normally regulates how cells respond to stress, but when overactive it enables cancer cells to withstand the damaging effects of chemotherapy.
Using CRISPR/Cas9 technology, the team engineered lung cancer cells to carry the R34G mutation, then knocked out NRF2 completely.
Using CRISPR/Cas9 technology, the team engineered lung cancer cells to carry the R34G mutation, then knocked out NRF2 completely. This intervention restored sensitivity to chemotherapy drugs including carboplatin and paclitaxel. Animal models treated with CRISPR-edited cells also demonstrated slower tumour growth and stronger responses to chemotherapy.
“This work brings transformational change to how we think about treating resistant cancers,” said Dr Eric Kmiec, senior author of the study and Executive Director of the Gene Editing Institute. “Instead of developing entirely new drugs, we are using gene editing to make existing ones effective again.”
High precision and clinical promise
One of the study’s most encouraging findings is that editing only 20-40 percent of tumour cells was enough to improve chemotherapy response and shrink tumours – a crucial insight for real-world treatment, where complete gene editing may be difficult.
For delivery, the research team used lipid nanoparticles (LNPs), a non-viral method known for high efficiency and low risk of unintended genetic edits. Sequencing results confirmed that the CRISPR edits were very specific to the NRF2 mutation.
"The power of this CRISPR therapy lies in its precision. It's like an arrow that hits only the bullseye," said Banas. "This level of specificity with minimal unanticipated genomic side effects offers real hope for the cancer patients who could one day receive this treatment."
Topics
- Cancer
- Cancer
- Cell & Gene Therapy
- Chemotherapy
- ChristianaCare’s Gene Editing Institute
- CRISPR
- Dr Eric Kmiec (Executive Director of the Gene Editing Institute)
- Dr Kelly Banas (Associate Director of Research at the Gene Editing Institute)
- Drug Development
- Drug Discovery Processes
- Gene Editing Technologies
- Gene Therapy
- In Vivo Testing
- Molecular Biology
- Oncology
- Precision Medicine
- Translational Science