Researchers have developed a novel CRISPR method that evades the immune system in mice, allowing scientists to study tumour growth and metastasis more accurately.
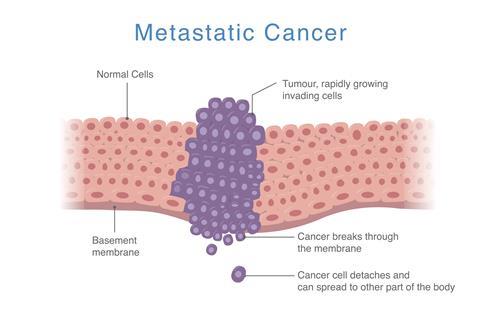
Scientists at ETH Zurich have announced a new method to improve cancer research in mice by making CRISPR/Cas9 invisible to the immune system. The innovation could accelerate the discovery of new therapies for metastatic cancers.
Immune system complicates cancer research
The immune system plays a crucial role in fighting tumours and metastases. This means it is essential to conduct cancer research in mouse models with as natural an immune system as possible – which is easier said than done.
CRISPR/Cas9 technology allows researchers to switch off hundreds of genes in tumour cells, revealing which genes influence cancer development and spread. When these modified cells are transplanted into mice, scientists can identify potential targets for new therapies.
However, the issue is that the CRISPR/Cas9 system is derived primarily from bacteria, which means the mouse immune system recognises it as foreign and attacks it. Researchers suspected this immune reaction could distort experimental results.
Bacterial components interfere
The team led by Professor Nicola Aceto, a molecular oncology expert at ETH Zurich, investigated how bacterial CRISPR components affect tumour growth in mice.
We were surprised at how significantly this can distort the results of CRISPR screens.
They found that tumour cells containing CRISPR/Cas9 were often rejected by the immune system and formed fewer metastases.
“We were surprised at how significantly this can distort the results of CRISPR screens,” said Massimo Saini, first author of the study and ETH Pioneer Fellow.
A cloak of invisibility for gene editing
To address this problem, the ETH researchers developed a new method that triggers almost no immune response. Tumour cells are briefly exposed to the Cas9 gene-editing enzyme, and only cells in which a gene has been successfully silenced are selected. These cells no longer contain Cas9 or other immune-triggering elements.
We have developed a method for performing CRISPR screens in mice with intact immune systems, without incurring any undesirable side effects.
The researchers also replaced standard reporter genes – which help track modified cells – with a version that similar to naturally occurring mouse proteins. This modification allows the cells to remain undetected by the immune system.
“We have developed a method for performing CRISPR screens in mice with intact immune systems, without incurring any undesirable side effects,” said Professor Aceto. He added that the system is versatile and can be used in humanised mice. The approach could also be applied to personalised medicine or autoimmune disease research.
New targets for metastasis
The CRISPR system identified two genes, AMH and AMHR2, that when silenced, reduced metastases in mouse models of breast cancer. Further analysis showed that high AMH protein levels in patients’ tumours were linked to more frequent relapses and higher mortality, highlighting the clinical importance of the signalling pathway.
“The significance of this signalling pathway has been underestimated,” said Professor Aceto. “Thanks to CRISPR in stealth mode, we are now able to uncover connections that were previously hidden.”