IVF babies: Easy as 1, 2…3?
Posted: 3 November 2016 | Niamh Louise Marriott, Digital Content Producer | No comments yet
The ethics of three parent babies has been widely debated – should it be used to save children from deadly mitochondrial diseases or are scientists “playing God”? Here’s everything you need to know to decide…

In 2015, the UK government controversially approved three parent IVF, becoming the first country to legally investigate mitochondirial donation, following approval of The Human Fertilisation and Embryology Regulations. In September of this year, the first three parent child was born via mitochondiral donation – a special form of in vitro fertilisation (IVF) in which a future baby’s mitochondrial DNA comes from a third party, and is combined with mother and father DNA before being implanted into the mother’s womb.
This technology is rapidly progressing, causing widespread discussion on the ethics and social concerns of such a procedure. Although the donor egg is said to contribute only 1% to the genetic makeup of the child, when examining the genetic material of these children there are still three identifiable genetic parents, which opponents to the technology argue could cause the child psychological and physical damage, with many insisting that scientists are “playing God”.
How three parent babies are made
There are two different types; spindle transfer and pronuclear transfer which are shown in the graphics below.
Spindle transfer


This technique takes the unfertilised mother’s egg (containing abnormal mitochondria) and the unfertilised donor’s egg (with healthy mitochondria), removes the spindle and other chromosomes from the mother’s and transfers them to the donated egg. This reconstituted egg is then fertilised with sperm from the father.
Pronuclear transfer
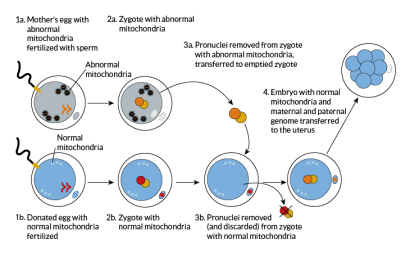

In this case, both the mother’s egg (containing abnormal mitochondria) and the donated egg (with normal mitochondria) are fertilised with the father’s sperm before the mother’s pronuclei is removed and transferred into the donor’s egg. It is then implanted into the mother’s uterus.
“This is great news and a huge deal,” says Dusko Ilic, King’s College London. “It’s revolutionary.”
The first three parent baby was born via spindle transfer. Watch the video below to find out how!
So why do we need this procedure in the first place?
Every year, about one in 200 children are born with faults in their mitochondrial DNA, which can cause diseases. Mitochondria are small structures that sit inside cells providing them with energy.
How do the diseases affect people?
Mitochondrial diseases tend to strike in childhood and get steadily worse. They often prove fatal before adulthood. The parts of the body that need most energy are worst affected: the brain, muscles, heart and liver. Conditions include Leigh’s disease, progressive infantile poliodystrophy and Barth syndrome.

Faulty mitochondria have been linked to epilepsy and diabetes
Faulty mitochondria have also been linked to more common medical problems, including Parkinson’s, deafness, failing eyesight, epilepsy and diabetes.
OPINION: Commenting after the government approved three parent IVF in 2015, Sally Cheshire, chairwoman of the Human Fertilisation and Embryology Authority, said, “Britain is the first country in the world to permit this treatment, and it is a testament to the scientific expertise and well-respected regulatory regime that exists across the UK that Parliament has felt able to approve it. The HFEA now have to develop a robust licensing process, which takes into account on a case by case basis the technical and ethical complexities of such treatments to ensure that any children born have the best chance of a healthy life.”
Ethical concerns
Mitochondria are not completely understood, and the DNA they hold might affect people’s traits in unknown ways, leading some scientists to want further research before the procedures become common place. Several prominent religious groups have spoken out; The Church of England says it is not opposed in principle, but wants to see more scientific research and debate on the ethics, safety and efficacy.Mitochondrial transfer passes on genetic changes from one generation to another. That raises ethical concerns because any unexpected problems caused by the procedure could affect people who are not yet born, and so cannot give their consent to have the treatment.
Back to basics: Two parent in vitro fertilisation process:
- Suppressing the natural menstrual cycle
Can make medicines used in the next stages of treatment more effective, can be taken as a daily injection or as a nasal spray.
- Boosting the egg supply
A daily dose of follicle stimulating hormone (FSH), a fertility hormone, is introduced.
Benefits of FSH: FSH increases the number of eggs your ovaries produce meaning more eggs can be collected and fertilised, giving a greater choice of embryos to use.
- Monitoring progress and final injections
Vaginal ultrasound scans to monitor your ovaries and, in some cases, blood tests are used to monitor the progress of the treatment. About 34-38 hours before the eggs are due to be collected, a final injection helps them to mature.
- Collecting the eggs
After sedation, the eggs are collected using a needle passed through the vagina into each ovary. This is completed with ultrasound guidance and the entire procedure takes about 20 minutes. Some women experience cramps and small vaginal bleeding after this procedure.
- Fertilising the eggs
After the eggs have been collected they are mixed with the partnering sperm in a laboratory. Then, after 16-20 hours, they are checked for fertilisation. The best one or two embryos are transferred to the womb within six days.
- Embryo transfer
The embryos are transferred into the womb via catheter. The number of embryos that will be discussed before treatment starts and usually depends on age.
- Women under 37 in their 1st and 2nd IVF cycles should only have a single embryo transfer. Doctors should only consider using two embryos if no top-quality embryos are available. In the third IVF cycle, no more than two embryos should be transferred.
- Women aged 37-39 years in the 1st and 2nd full IVF cycles should also have single embryo transfer if there are one or more top-quality embryos, and double embryo transfer should only be considered if there are no top-quality embryos.
- Women aged 40-42 years may have a double embryo transfer.
Criteria for IVF referral
The National Institute for Health and Care Excellence (NICE) published fertility guidelines recommending who should have access to IVF treatment. According to their site, IVF should be offered to women under 40 years of age who have been trying to get pregnant through regular unprotected sex for two years, or who have had 12 cycles of artificial insemination. The final cut off point for women is 42.
However, the final decision about who can have NHS-funded IVF in England is made by local Clinical Commissioning Groups (CCGs), and their criteria may be stricter than those recommended by NICE.


IVF can be available from a private clinic and whilst costs vary, one cycle of treatment can set you back over £5,000.
The full list of guidelines can be found here
Chance of success
The graph below shows that the average IVF success rates using own eggs starts to drop at about 30 and drops faster in the mid 30s and early 40s. This drop is caused by decreasing egg quantity and quality. Live births are rare at age 44 and above using the female partner’s eggs.
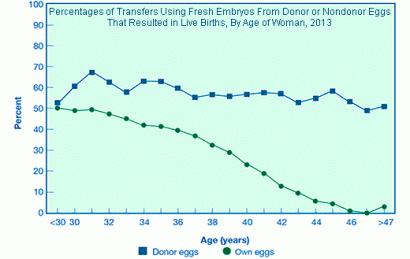

The green line shows IVF success rates by age using the woman’s own eggs and the blue line shows success rates using donor eggs by age of the recipient woman.
In 2013 (the year for which the most recent data is available) women having IVF using fresh embryos created with their own fresh eggs, the percentages of cycles started that resulted in a live birth were:
- 2% for women aged under 35
- 7% for women aged between 35–37
- 8% for women aged between 38–39
- 6% for women aged between 40–42
- 0% for women aged between 43–44
- 9% for women aged 45 and over
Age chance stats taken from here.


There are serious risks associated with IVF treatment including multiple births
Risks of IVF
Few IVF treatments results in full term pregnancy and it can be both physically and emotionally demanding.
There are a number of health risks involved, including:
- side effects from the medications used during treatment, such as hot flushes and headaches
- multiple births (such as twins or triplets) – this can be dangerous for both the mother and the children
- an ectopic pregnancy – where the embryo implants in the fallopian tubes, rather than in the womb
- ovarian hyperstimulation syndrome (OHSS) – where too many eggs develop in the ovaries
National Fertility Awareness Week is Monday 31st October to Sunday 6th November 2016
#HiddenFaces Never being called mum; never feeling like a real woman; that is the pain of never: Jessica Hepburn
Related topics
in vitro fertilisation (IVF), intra-cytoplasmic sperm injection, mitochondirial donation
Related organisations
The National Institute for Health and Care Excellence (NICE)



