Scientists have grown the first multi-regional “mini-stomach” in the lab, creating a new way to study rare genetic stomach diseases and help to develop new treatments for digestive conditions.
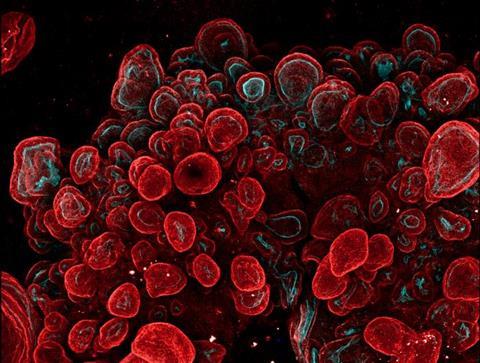
A University College London study has developed a lab-grown “mini-stomach” organoid that can replicate the three main regions of the human stomach. Known as a multi-regional assembloid, it contains the fundic, body and antrum regions of the stomach. These regions combine to form the inner lining of the stomach – called the mucosa – which is vital for acid digestion, protection against self-digestion and hormone regulation.
How the mini-stomach was created
The team described how they isolated stem cells from patient stomach samples and grew them under specialised laboratory conditions in petri dishes. This process produced organoids – or mini-stomachs – that mimic the behaviour of a human stomach.
The researchers first cultivated separate organoids for each of the three main stomach regions. They then combined them into a single “assembloid” version – which had never been achieved before.
The team discovered that each component retained the characteristics of the region it was derived from and communicated with the other parts in the same way a full-sized stomach does. The assembloids were also capable of key functions of digestion, such as producing stomach acid.

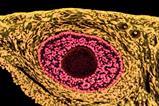
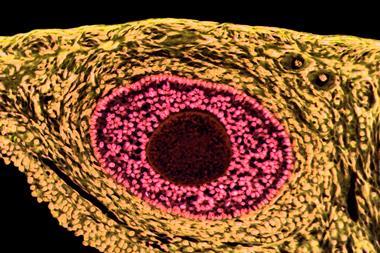
Immunofluorescence images of a gastric body assembloid showing integrin-b4 in red and f-actin in cyan. Credit: B. Jones, G. Benedetti et al., Nature Biomedical Engineering.[/caption]
Modelling rare genetic stomach disease
The researchers then applied the technique to study a very rare genetic stomach disorder, opening the possibility of using the model for more common gastric diseases that remain poorly understood.
“Traditional organoids and animal models fail to replicate the regional architecture and functional diversity of the human stomach,” said senior author Dr Giovanni Giobbe of UCL Great Ormond Street Institute of Child Health. “Recent advances in gastric assembloid technologies offer the potential to model region-specific physiology and disease phenotypes in vitro. Our multi-regional gastric assembloids replicate the antrum-body-fundus structure and function, including acid secretion, and are uniquely positioned to unravel disease mechanisms in rare gastric disorders.”
Targeting PMM2-HIPKD-IBD
After confirming the assembloid model worked, the team grew multi-regional mini-stomachs from the stem cells of children with Phosphomannomutase 2-associated Hyperinsulinism with Polycystic Kidney Disease and Inflammatory Bowel Disease (PMM2-HIPKD-IBD). Children with this condition experience kidney and blood sugar problems and unusual stomach changes known as antral foveolar hyperplasia, which can lead to bleeding, inflammation or increased cancer risk.
The mini-stomachs allowed researchers to test both the underlying cause of the disorder and potential treatments. This approach could speed up clinical approval of therapies for PMM2-HIPKD-IBD by providing robust patient-derived data.
“This is an important development towards a personalised treatment for patients with this rare and complicated genetic condition,” said co-author Dr Kelsey Jones, Consultant in Paediatric Gastroenterology at GOSH. “It provides an example of how working with patients to understand the scientific basis of disease can lead to real benefits for them and their families.”
Funding and future work
The research was funded by the National Institute for Health and Care Research (NIHR) Great Ormond Street Hospital (GOSH) Biomedical Research Centre, with support from the Oak Foundation and GOSH Charity. GOSH Charity will now help continue the work, including testing repurposed drugs to treat PMM2-HIPKD-IBD.
“This innovative work using miniature stomachs showcases how researchers in NIHR infrastructure are driving the UK’s life sciences edge," said Professor Marian Knight, Scientific Director for NIHR Infrastructure. "Working with patients living with rare diseases has led to the discovery of potentially life-changing treatments. If this experimental approach can be used for other conditions, it will bring hope to many patients struggling to get the treatments they need.”
Topics
- 3D Cell Cultures
- Analytical Techniques
- Biotechnology & Bioengineering
- digestive disorders
- Disease Research
- Dr Giovanni Giobbe (UCL Great Ormond Street Institute of Child Health)
- Dr Kelsey Jones (Consultant in Paediatric Gastroenterology at GOSH)
- Drug Discovery Processes
- Ex Vivo Models
- Great Ormond Street Hospital (GOSH)
- High-Throughput Screening (HTS)
- Imaging & Diagnostics
- In Vitro Testing
- Microscopy
- Molecular Biology
- Neurological disorders
- Organoids
- Pathology & Molecular Medicine
- Personalised Medicine
- Professor Marian Knight (Scientific Director for NIHR Infrastructure)
- Regenerative Medicine
- Regenerative Medicine
- Regenerative Medicine dupe
- Stem Cells
- the Oak Foundation
- Translational Science
- University College London