Researchers identify promising drug combination for tuberculosis
Posted: 29 March 2016 | Victoria White | No comments yet
Researchers used feedback system control to quickly narrow combinations of 14 different tuberculosis drugs with five different doses into several promising combination treatments…
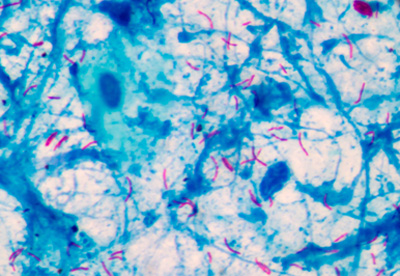

Researchers have made important steps towards a more effective treatment for tuberculosis.
Combination therapy is a clinical standard for many major diseases. However, the number of potential combinations of different drugs and dose levels can be in the billions, making the prospect of choosing the best one seem daunting.
In the study, researchers from UCLA and Shanghai Jiao Tong University used a technique called feedback system control to study cells infected with the bacteria that cause tuberculosis. They quickly narrowed combinations of 14 different tuberculosis drugs with five different doses into several promising combination treatments that kill the bacteria that cause tuberculosis much faster than the standard regimen used to treat tuberculosis.
Commenting on the research, Chih-Ming Ho, the study’s principal investigator, said: “Designing a drug combination with optimized drug-dose ratios has, until now, been virtually impossible. Feedback system control technology demonstrated it can pinpoint these best possible ratios for a wide spectrum of diseases.”
“If our findings are confirmed in human studies, the new drug regimens that we have identified should dramatically shorten the time needed to treat tuberculosis,” added Dr Marcus Horwitz, a distinguished professor of medicine and microbiology, immunology and molecular genetics at the UCLA David Geffen School of Medicine. “This will increase the likelihood of successful treatment and decrease the likelihood of patients developing drug-resistant tuberculosis. A highly successful and rapid treatment may hasten the eventual eradication of tuberculosis.”
Researchers identified the ideal drug-dose combinations after four rounds of testing
The study’s researchers infected macrophages with a highly virulent strain of TB. The bacteria were engineered to fluoresce while they lived, so drug regimens that killed the bacteria eliminated the fluorescence.
Feedback system control quickly eliminates potential dead ends and automatically readjusts drug-dose combinations to zero in on the most effective ones, saving a tremendous amount of time and effort. This allowed the researchers to identify ideal drug-dose combinations after just four rounds of testing, with about 125 tests per round.
The research team also found that two major TB drugs, isoniazid and rifampin, were counterproductive when combined with other drugs. Another drug, clofazimine, which is not usually used in tuberculosis treatments, was included in most of the promising combinations.
The researchers have also completed an animal study. That study’s results have prompted human trials of one promising combination, and plans are underway to test another.
Related conditions
Tuberculosis (TB)
Related organisations
Shanghai Jiao Tong University, UCLA



