Possible new target for psoriasis identified
Posted: 13 June 2016 | Victoria White, Digital Content Producer | No comments yet
A small protein in the skin called Rac1 appears to link well-known environmental triggers of the disease with a genetic predisposition to the condition…
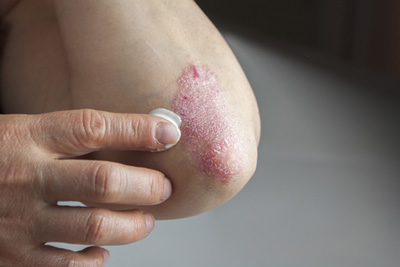

Researchers at the Stanford University School of Medicine have identified a new molecular target for potential therapies for psoriasis.
A small protein in the skin called Rac1, which is involved in wound repair, appears to link well-known environmental triggers of the disease with a genetic predisposition to the condition. It also sheds light on the interplay between the skin and the immune system that is responsible for disease flare-ups.
“Normally there’s a quiet, ongoing conversation between the epidermis and our immune system as they work together to fight disease such as infections,” explains Peter Marinkovich, MD, associate professor of dermatology. “In psoriasis, this has escalated into an uncontrollable shouting match that results in abnormal cellular proliferation, scaling and inflammation with no real effective therapies other than long-term immunosuppression. Targeting a protein in the skin, rather than quieting the immune system, could be a potential game changer for many patients and clinicians.”
About one of every 50 people in the world has psoriasis. Flare-ups can be triggered when skin is damaged and the epidermal cells become hypersensitive to growth signals. That’s why many people struggle with the condition on their elbows, knees and other areas of the body that tend to get roughed up. The disease can also be activated in susceptible people by the streptococcal bacteria that cause a sore throat.
The exact mechanisms by which these events trigger the disease are unknown, and most therapies focus on quieting the immune system’s side of the noisy conversation.
Mice exhibit psoriasis symptoms when Rac1 is activated
The Stanford researchers tried to find other options for patients by eavesdropping on the skin’s role in the disease process. That meant considering environmental triggers, which led them to a small molecule, called Rac1, known to play a role in both wound repair and in strep infection.
When activated, Rac1 is believed to promote the proliferation of cells in the epidermis, as well as send signals to activate the immune system. Under normal conditions, this is a necessary response to heal after an injury. But over-proliferation and over-inflammation could have detrimental effects. Interestingly, some genetic mutations that have been linked to psoriasis affect molecules that are involved in many of the same signalling pathways as Rac1.
The researchers consistently found that Rac1 was highly activated in biopsies of psoriatic skin from 20 people with the condition. When they artificially activated Rac1 in the skin of laboratory mice, the animals exhibited similar symptoms as human patients.
“They had scaling of the skin and arthritis in their joints that precisely mimics what we’ve seen in the clinic,” Marinkovich said. The effect was abolished, however, in mice engineered to lack T cells – further confirming the immune system’s role in the disorder.
Finally, blocking the activity of Rac1 in patches of psoriatic human skin that had been transplanted onto the backs of mice reversed the skin hyperplasia and reduced the recruitment of immune molecules known as cytokines to the transplanted patch.
Marinkovich commented: “Now we’ve learned that targeting Rac1 activation in the skin, rather than the immune system’s role in the disease, may be a way to treat the disease without needing to suppress the immune system.”
Marinkovich and his colleagues plan to continue their study of what causes Rac1 activation in the epidermis.
Related topics
Molecular Targets
Related conditions
Psoriasis
Related organisations
Stanford University School of Medicine