A previously unknown genetic disorder causing premature ageing and neurological decline has been identified by scientists using advanced genome sequencing and stem cell models to find its underlying mechanisms.
Scientists at the Sanford Burnham Prebys Medical Discovery Institute and an international team of collaborators have identified a previously unknown genetic disease characterised by premature ageing and neurological decline.
Their research is the first study to combine genome sequencing with cellular reprogramming to pinpoint the causative mutation and explore how it drives disease.
Unusual symptoms point to unknown condition
The discovery began when clinicians identified a family in which teenage members showed signs typically associated with progeria syndromes, including premature greying of hair. However, the patients also exhibited symptoms not usually seen in such conditions.
The discovery began when clinicians identified a family in which teenage members showed signs typically associated with progeria syndromes.
“Our collaborator identified a family of patients whose teenaged members had whitening hairs and other characteristics associated with premature ageing conditions known as progeria syndromes,” said Director of the Center for Neurologic Diseases at Sanford Burnham Prebys and a senior author in the study, Dr Su-Chun Zhang. “Cognitive functions are often well preserved in these conditions, however, so it was clear from the patients’ progressive loss of motor skills and neurological and intellectual deficits that this was an unknown disease.”
Pinpointing a genetic cause
Using genome sequencing alongside mapping techniques for recessive traits, the researchers traced the condition to a mutation in the IVNS1ABP gene. This gene encodes a protein known to bind influenza virus components but had not previously been linked to ageing or neurological disease.
“Relatively little research has been done on this gene and protein, and no one has ever linked them to the biology of ageing, premature ageing diseases or neuropathy,” said Staff Scientist at Sanford Burnham Prebys and first author, Dr Fang Yuan. “It was a mystery in many ways and one we were determined to solve.”
Stem cell models reveal cellular damage
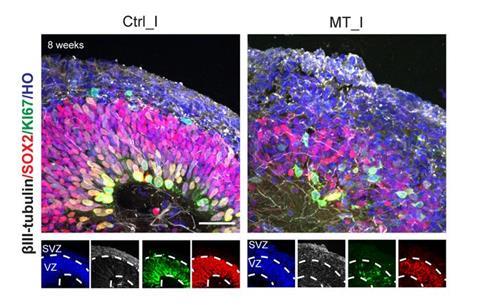
To understand how the mutation affects cells, the team reprogrammed skin cells from patients into induced pluripotent stem cells (iPSCs) and then into neural progenitor cells. These cells retained the genetic mutation, allowing detailed study in the laboratory.
“Under the microscope, we found that the patient-derived cells with the mutation grow much slower compared to the control group reprogrammed from a sibling without the disease,” said Zhang.
Further investigation showed that the affected cells had entered cellular senescence
Further investigation showed that the affected cells had entered cellular senescence, a state in which cells stop dividing. Researchers identified multiple markers of DNA damage along with increased levels of a gene linked to this process.
“To narrow in on what was causing these cells to become senescent, we ran follow-up experiments showing that DNA damage was occurring during cell division and we saw that it could be severe enough to cause cell death,” said Yuan.
Faulty cell division mechanism uncovered
Although the IVNS1ABP gene had no known direct role in cell division, the team found evidence that it interacts with proteins involved in a key structural component of cells, called actin.
“During cell division, the actin filament needs to form an anchoring structure and it usually forms a very round and even ring structure,” said Zhang. “But in the mutant cells, the altered actin forms a shrunken and irregularly shaped ring so cells are not pulled apart in a symmetrical way and suffer damage.
“When these actin dynamics are altered, the cell cannot perform cell division at the right time and in the right place,” Yuan added.
Hope for future treatments
Encouragingly, the researchers found that treating the cells with compounds that stabilise actin structures improved normal cell division.
“This research highlights the potential of using cellular reprogramming and patient-derived stem cell models to study rare and unknown diseases,” said Zhang.
This research highlights the potential of using cellular reprogramming and patient-derived stem cell models to study rare and unknown diseases
The researchers have demonstrated that correcting certain steps in the molecular processes can repair some of the cellular defects – at least in the lab-grown cell models.
They emphasised, however, that further studies using an animal model are needed to confirm the findings but the work already highlights the power of this approach for identifying new diseases and exploring potential treatments.















No comments yet