Stanford researchers have cured Type 1 diabetes in mice using a combination of blood stem cell and pancreatic islet cell transplants.
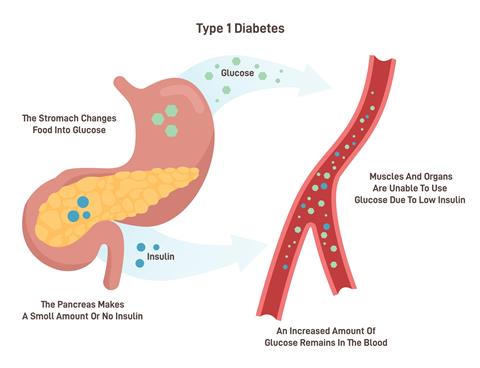
Researchers at Stanford Medicine have successfully prevented or cured Type 1 diabetes in mice using a combination of blood stem cell and pancreatic islet cell transplants from immunologically mismatched donors. The study offers scientists brand new insights for potential future treatments in humans.
Type 1 diabetes develops when the immune system mistakenly destroys insulin-producing islet cells in the pancreas. Traditional treatments involve lifelong insulin therapy, but this new approach prevents disease progression and eliminates the need for immune-suppressing drugs.
Hybrid immune system protects against disease
“The possibility of translating these findings into humans is very exciting,” said Dr Seung K. Kim, MD, the KM Mulberry Professor and a professor of developmental biology, gerontology, endocrinology and metabolism. “The key steps in our study – which result in animals with a hybrid immune system containing cells from both the donor and the recipient – are already being used in the clinic for other conditions. We believe this approach will be transformative for people with Type 1 diabetes or other autoimmune diseases, as well as for those who need solid organ transplants.”
In the experiments, none of the mice developed graft-versus-host disease, a serious complication where donor immune cells attack the recipient’s tissues. The native immune system also no longer destroyed islet cells after transplantation, demonstrating long-lasting protection.
Building on previous research
The study builds on work from 2022, when Kim and colleagues cured diabetes in mice by destroying insulin-producing cells with toxins. They followed this up with a combination of low-dose radiation, immune-targeting antibodies and donor cell transplantation.
Just like in human Type 1 diabetes, the diabetes that occurs in these mice results from an immune system that spontaneously attacks the insulin-producing beta cells in pancreatic islets.
“This study tackled a more complex problem: curing or preventing diabetes caused by autoimmunity,” Kim explained. “Just like in human Type 1 diabetes, the diabetes that occurs in these mice results from an immune system that spontaneously attacks the insulin-producing beta cells in pancreatic islets. We need to not only replace the islets that have been lost but also reset the recipient’s immune system to prevent ongoing islet cell destruction. Creating a hybrid immune system accomplishes both goals.”
By adding a drug already used to treat autoimmune diseases to their pre-transplant regimen, the team achieved a hybrid immune system in all 19 animals, preventing Type 1 diabetes. Nine mice with established diabetes were completely cured following the combined blood stem cell and islet transplant.
Safer stem cell transplants
The approach builds on previous research that demonstrated a partially matched bone marrow transplant could create a hybrid immune system. This allowed long-term acceptance of kidney transplants without lifelong immune suppression.
“Based on many years of basic research by us and others, we know that blood stem cell transplants could also be beneficial for a wide range of autoimmune diseases,” Shizuru said. “The challenge has been to devise a more benign pre-treatment process, diminishing risk to the point that patients suffering from an autoimmune deficiency that may not be immediately life-threatening would feel comfortable undergoing the treatment.”
What is next?
Donor islets can only be obtained after death, and blood stem cells must come from the same donor. To try and overcome this, researchers are now exploring ways to generate islet cells in the laboratory and improve transplant survival.
Researchers are now exploring ways to generate islet cells in the laboratory and improve transplant survival.
“The ability to reset the immune system safely to permit durable organ replacement could rapidly lead to great medical advances,” Kim said.
Beyond diabetes, this approach could extend to autoimmune diseases such as rheumatoid arthritis and lupus, as well as non-cancerous blood disorders like sickle cell anaemia.
Topics
- Analytical Techniques
- Autoimmune disease
- Biotherapeutics
- Cell & Gene Therapy
- Disease Research
- Dr Seung K. Kim MD (the KM Mulberry Professor and a professor of developmental biology gerontology endocrinology and metabolism)
- Genomics & Sequencing
- Immunoassays
- Immunogenicity Testing
- Immunology
- In Vivo Testing
- Metabolic disorders
- Regenerative Medicine
- Stanford Medicine
- Stem Cells
- Translational Science