Scientists stabilise HIV structure and design potential vaccine candidates
Posted: 29 June 2016 | Victoria White, Digital Content Producer | No comments yet
Scientists have described a strategy to stabilise an important HIV structure and potentially create HIV lookalikes for large-scale vaccine production…
In a feat of bioengineering, the team designed nanoparticles that could mimic HIV. CREDIT: The Scripps Research Institute
Scientists from The Scripps Research Institute (TSRI) have described a strategy to stabilise an important HIV structure and potentially create HIV lookalikes for large-scale vaccine production.
Using this new knowledge, in a second study, TSRI scientists have engineered novel nanoparticles as vaccine candidates.
“This is a big accomplishment in terms of engineering and design,” said TSRI biologist Jiang Zhu.
Zhu co-led the first study with Ian Wilson, Hansen Professor of Structural Biology and chair of the Department of Integrative Structural and Computational Biology at TSRI, and co-led the second with TSRI Associate Professor Andrew Ward.
In the first study, Zhu and researcher Leo Kong built on previous structural studies from the Ward and Wilson labs to investigate a trait called “metastability”. Metastability describes the tense state of the HIV Envelope glycoprotein (Env) trimer when it is poised like a loaded spring to undergo the dramatic changes that allow the virus to enter cells.
The problems of metastability
Metastability poses a problem for scientists who want to create a precise image of this viral target and see what the human immune system is up against. Metastability also stands in the way of naturally occurring immunity and vaccine production. For the adaptive immune system to work in either case, it needs to recognise a functional, stable version of a virus’s proteins – a sort of mugshot – so it can produce antibodies and attack the actual virus upon encountering it.
Unfortunately, because of the virus’s metastability, or shape-shifting tendency, structures of HIV’s proteins have proven difficult to establish for use in vaccine design. The Ward and Wilson groups at TSRI have previously determined cryo-EM and x-ray structures for other Env constructs; however, current methods to stabilise Env in one strain of HIV won’t necessarily stabilise it in another, making it hard to design an arsenal of Env proteins to help elicit “broadly neutralising antibodies” that could fight many types of HIV.
To advance the vaccine effort, TSRI researchers wanted to track down the root cause of metastability, and Jiang and Kong hypothesised that altering a key region of Env would improve its overall properties.
They hypothesised that a region of the Env called HR1 could be linked to metastability.

(L to R) Jiang Zhu, Charles Morris (back), Parisa Azadnia and Linling He.
“The HR1 basically resembles a highly bent twig that is ready to spring back straight,” said Kong. “This small bend in the HR1 region is likely ground zero for metastability. In most published Env structures, this region appears disordered when mutated or loosely packed when in its native form. From these observations, it seemed reasonable that rewiring the HR1 bend could greatly stabilise Env.”
Indeed, when the scientists tweaked HIV’s genetic sequence, they were able to shorten the HR1 region, preventing its transformation and keeping the rest of the structure stable.
“We’ve figured out one of the fundamental reasons why HIV is metastable,” said Zhu.
The researchers then demonstrated that their stabilised Env trimers also almost perfectly mimicked the structure of the real HIV trimer, suggesting they could be useful in vaccines.
Nanoparticles that mimic HIV
In the second study, the researchers looked into designing nanoparticles that could mimic HIV.
Nanoparticles provide the backbone of successful vaccines against human papillomavirus (HPV), hepatitis B and hepatitis E. These nanoparticles are called virus-like particles (VLPs) and are hollow shells of other proteins found in nature. Scientists have found that they can add viral proteins to the outside of a shell, creating a phony virus. The imposter then prompts the body to produce antibodies for long-term protection against the real virus.
But as Zhu and his colleagues focused on creating HIV-like VLPs, the Env trimer, once again, presented a challenge.
The trimer is made of three subunits that come together to form a base with a crown shape on top. The top of the crown is where the tips of the three subunits meet.
Scientists have found that the immune system cannot produce broadly neutralising antibodies when a vaccine contains only one part of the trimer. The immune system needs to see intact HIV proteins – also called antigens when they stimulate the immune system to create antibodies–in their native trimeric context.
Fusing a trimeric HIV-1 antigen to a nanoparticle
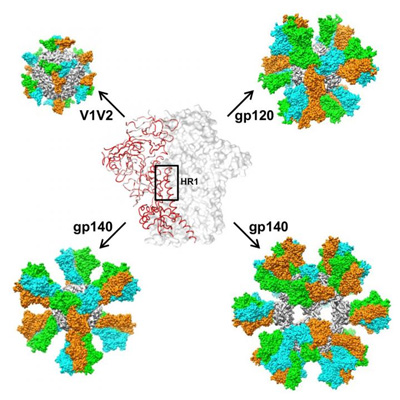
To construct an artificial virus, in the new study the researchers added HIV trimers to nanoparticles that naturally lock their own subunits together in clusters of three. As the three subunits come together, the researchers hypothesised, they could bring the HIV antigens together to form a trimer.
“Our idea was to ‘fuse’ a trimeric HIV-1 antigen to a nanoparticle subunit, so when the subunits ‘self-assemble’ they bring three attached HIV-1 antigens together,” said TSRI Staff Scientist Linling He.
It was a feat of geometry and engineering – and it worked. “It has been really challenging to properly present HIV Env on nanoparticles while keeping its natural trimeric form -but we did it,” said Zhu, “Multiple copies of Env are now displayed on the nanoparticle surface, just like what a real virus would do.”
The team then tested different nanoparticles and versions of the trimer, including one based on the stabilised Env in the first study, to find the best combinations. Six designs worked well in laboratory tests and now await trials in animal models.
Related conditions
HIV
Related organisations
The Scripps Research Institute (TSRI)


