Researchers gain insight into how brain tissue is impacted differently by genetic problems compared to the rest of the body.

Most people have the same genetic information in every cell of their body. However, usually during foetal development, people can develop two or more genetically diverse set of cells. Known as mosaicism, occasionally one of those groups of cells has genetic changes that may cause disorders or diseases.
Previous research has shown that mosaicism in the brain is an important contributor to epilepsy, so neurologists, neurosurgeons and genomic experts have collaborated to assess mosaicism in brain tissues resected during epilepsy surgery.
Scientists from Nationwide Children’s Hospital discovered an alternate origin of brain mosaicism in some children with focal epilepsy. Dr Adam Ostendorf, a paediatric neurologist at Nationwide Children’s Hospital and an author of the study said: “About one in every 26 people will have epilepsy at some point in their lives. The causes are incredibly diverse, and a mystery in over half of people with epilepsy.”
Drug-resistant seizures occur in about a third of epileptic children which significantly affects their quality of life, safety, and developmental outcomes. Seizure onset, especially in the child population, is related to specific risk factors like positive family history, fever, infections, neurological comorbidity, premature birth, mother’s alcohol abuse, and smoking in pregnancy.1 Dr Tracy Bedrosian, principial investigator in the Steve and Cindy Rasmussen Institute for Genomic Medicine at Nationwide Children’s Hospital, Assistant Professor of Paediatrics at The Ohio State University College of Medicine, and senior author of the study said: “We were motivated to study the genetic causes of drug-resistant epilepsy so future research might be able to develop more effective treatments.”
The scientists performed a genetic analysis of brain tissue, blood and buccal (epithelial) cells. Tissue samples were taken from six patients, aged two months to seven months, who underwent epilepsy surgery. The brain samples showed that some of the cells in the brain tissue, including astrocytes, had extra copies of chromosome 1q compared to the normal tissue. The blood and buccal cells did not have any cells with extra copies.
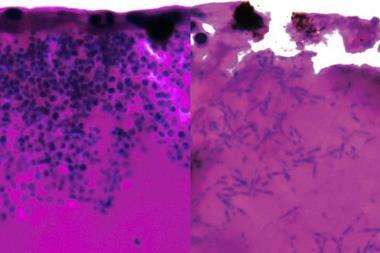
Markedly, astrocytes carrying the extra 1q displayed distinct gene expression signatures and histopathologic differences like hyaline inclusions, which supports the association of chromosome 1q gains with astrocytic inclusions in epilepsy.
Dr Bedrosian explained: “From a practical standpoint, in neurosurgical cases of focal epilepsy where we see certain histopathological signs, namely hyaline astrocytic inclusions, we can suspect the underlying genetic etiology is chromosome 1q gain.”
However, that etiology was not the only finding in the study. “The surprising finding was that the genetic alteration (chromosome 1q gains) was inherited in some of the patients, even though it was only found in a mosaic pattern within brain tissue,” Dr Bedrosian added. “This finding was a serendipitous observation that led us down a path to discover a novel mechanism for brain mosaicism.”
In five of the six patients, the analysis indicated that the extra chromosome copies were maternally derived, meaning they were present because of an error in the meiotic divisions that formed the egg. The analysis demonstrates that this error was corrected by cell repair mechanisms during embryonic or foetal development in most tissues (blood and buccal) but not in all brain cells.
Dr Katherine Miller, first author of the study and principal investigator in the Institute for Genomic Medicine, remarked: “We were able to genetically analyse blood from the mothers and then confirm that the extra chromosomal material was actually inherited, indicating a complex genetic phenomenon that resulted in the somatic mosaicism.”
“We were able to genetically analyse blood from the mothers and then confirm that the extra chromosomal material was actually inherited, indicating a complex genetic phenomenon that resulted in the somatic mosaicism.”
Mosaicism is typically expected to be the result of changes to the genetic material during foetal development, but this data exhibits an alternate mechanism of brain chromosomal mosaicism, where the increase in copy number was inherited as the result of a meiotic error. During foetal development, other cell lineages corrected these copy number gains making the copy number increase undetectable in blood and buccal cells.
“This work is incredibly exciting for two reasons,” noted Dr Ostendorf. “First, it links a recently identified cause to a pathology finding, furthering our understanding of how 1q gains cause unrelenting seizures. Second, it opens the door to new mechanisms of how brain tissue may be impacted by genetic problems differently than the rest of the body. Now, we have to reconsider how we look at genetic causes of epilepsy.”
“Recognising a meiotic origin for mosaicism is also important for genetic counselling and risk of recurrence,” explained Dr Bedrosian. “If the chromosome gain is in additional tissues, patients may face an increased risk of cancers. Additionally, the mother’s future pregnancies might also be affected.”
This study was published in Nature Genetics.
References
1 Astuto M, Minacapelli R, Minardi C, et al. Epilepsy in Children: From Diagnosis to Treatment with Focus on Emergency. Journal of Clinical Medicine [Internet]. 2019 January 2 [2023 October 24];8(1):39. Available from: https://www.mdpi.com/2077-0383/8/1/39