A new study could result in CTLA-4 inhibitors that promote antitumour responses without causing intestinal diseases, such as colitis.
Researchers from the University of Michigan and Takeda Pharmaceuticals have discovered a mechanism by which anti-CTLA-4 antibodies induce inflammatory toxicities during antitumour immune checkpoint inhibitor therapies. These findings may advance the development of next-generation CTLA-4 inhibitors that promote antitumour responses without triggering intestinal disease.
Cancer immunotherapies with immune checkpoint inhibitors are extensively used to promote antitumor immune responses in a variety of human cancers. However, they can lead to inflammatory toxicities known as immune-related adverse events (irAEs).
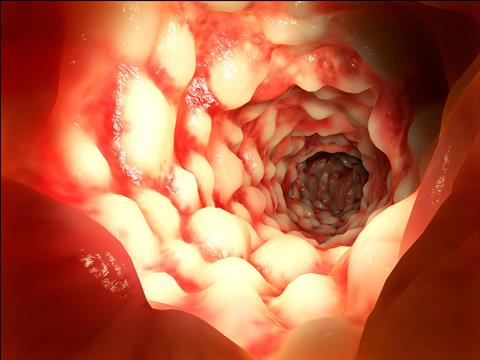
Colitis, the chronic intestinal disease characterised by inflammation of the colon’s inner lining, is a severe irAE. This can result in treatment discontinuation, especially in patients treated with antibodies targeting the checkpoint inhibitor protein CTLA-4.
Microbiota-reactive T cells trigger colitis in mice harbouring the microbiota of wild-caught mice following CTLA-4 blockade. Conventionally raised laboratory mice are highly resistant to intestinal inflammation after treatment with antibodies targeting immune checkpoints, so the immunological mechanisms and role of the gut microbiota underlying immune checkpoint blockade (ICB)-induced colitis in patients are not fully understood.
In the new study, Dr Bernard Lo, from the Department of Pathology and Rogel Cancer Center at the University of Michigan, and his colleagues, investigated whether mice harbouring a referenced gut microbiota originally derived from wild-caught mice (wild mouse microbiome-reconstituted or WildR mice) would be an improved model system for ICB-induced colitis.
Unlike conventionally raised specific pathogen-free mice, the authors found that WildR mice develop robust colitis after treatment with anti-CTLA-4 antibodies. Also, they saw that the inflamed tissues in these mice displayed multiple hallmark features of clinical ICB-associated colitis.
The results demonstrate that CTLA-4 blockade-induced colitis in mice is dependent on gut microbiota composition and that it is driven by unrestrained activation of a subset of the regulatory T cells in the gut by receptors recognising the Fc domain of the anti-CTLA-4 antibodies used in CTLA-4 ICB therapies.
The authors showed that anti-CTLA-4 nanobodies lacking the Fc domain can promote antitumor responses without inducing colitis, which could offer a strategy for mitigating gut IrAEs while preserving the antitumor effects of CTLA-4 blockade therapies.
The study was published in Science.