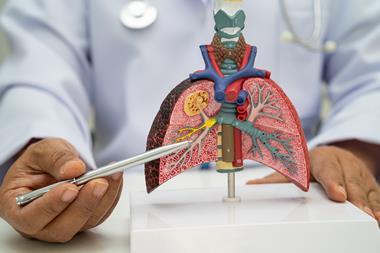
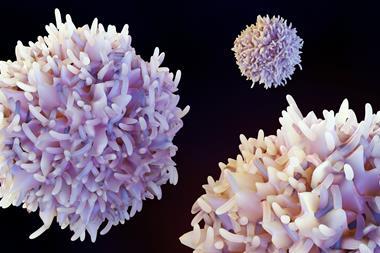
One treatment with the anti-TRBC1-SG3249 ADC combination saw cancer elimination within seven days in mouse models.
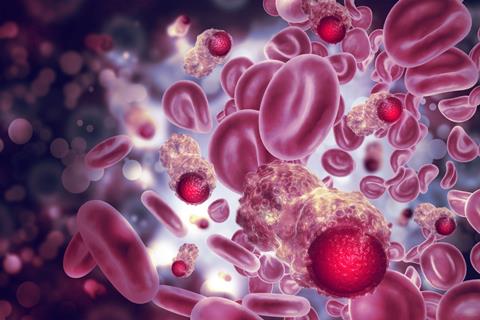
Researchers at the Johns Hopkins Kimmel Cancer Center and its Lidwig Center and Lustgarten Laboratory have developed a novel treatment for leukaemias and lymphomas that arise from immune system T cells. This treatment was effective at killing these cancers in mice bearing human T-cell tumours.
Around 100,000 patients each year worldwide are affected by T-cell leukaemias and lymphomas. Adults with relapsed T-cell cancers have limited therapeutic options and a five-year survival rate of seven to 38 percent, highlighting the requirement for new treatments.
Senior study author Dr Suman Paul, assistant professor of oncology at the Johns Hopkins University School of Medicine, explained: “Developing treatments for T-cell leukaemias and lymphomas is much more difficult than for leukaemias and lymphomas arising from immune system B cells.” Although effective therapies for B-cell cancers destroy both cancerous and noncancerous B cells, patients still do well. However, if a treatment destroys both normal and cancerous T cells, it will leave patients without a functioning immune system and at high risk of dying from infections.
“Not much drug development has happened in this space of T-cell leukaemias and lymphomas,” Dr Paul continued. “We need new therapies for these cancers, but whatever therapies we develop in the space have to be cancer-specific. We have to preserve some of the normal T cells and wipe out cancerous T cells at the same time.”
TRBC1
While normal T cells express a mix of TRBC1 and TRBC2, T-cell cancers express either TRBC1 or TRBC2. Therefore, selective targeting of TRBC1 can possibly eradicate the normal and cancerous T cells expressing TRBC1 while preserving normal T cells expressing TRBC2.
A recent clinical trial conducted elsewhere tried to target TRBC1 cancers using chimeric antigen receptor (CAR) T-cell therapy. Approved by the Food and Drug Administration (FDA), CAR T-cell therapies are used in several B-cell cancers. Despite this, after administering the TRBC1-targeting CAR T cell therapy in human patients, trial investigators reported that the CAR T cells were not persisting inside the patients. Such persistence is needed for effective cancer cell-killing. Investigating why, Dr Paul and his team discovered that the CAR T cells targeting TRBC1 could be killed by normal T cells, limiting their persistence.
This meant that the team attempted to target TRBC1 with the use of antibody-drug conjugates (ADCs) instead, trying two different formulations of ADCs in mouse models of T-cell cancers. Following a single injection of one formulation of the treatment, the cancers initially regressed but then recurred. After a single treatment with the anti-TRBC1-SG3249 ADC combination, the scientists observed signs of cancer elimination within seven days and the cancers were eventually undetectable, with no recurrences. Dr Paul stated: “The tumours didn’t come back, and we followed the mice for more than 200 days.”
The treatment eliminated the cancer while preserving half of the remaining normal T cells. “The residual normal T cells should be sufficient to maintain some immune system protection against infectious diseases,” Dr Paul said.
Currently, the researchers are working with an industry partner to conduct early-phase safety and efficacy trials in human patients.
This study was published in Nature.