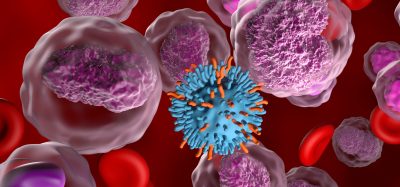
Immune cells the missing ingredient in new bladder cancer treatment
Posted: 24 July 2017 | Dr Zara Kassam (Drug Target Review) | No comments yet
New research offers a possible explanation for why a new type of cancer treatment hasn’t been working as expected against bladder cancer…

New research offers a possible explanation for why a new type of cancer treatment hasn’t been working as expected against bladder cancer.
In this study, a team of scientists from H3 Biomedicine headed by Dr Ping Zhu, found that some invasive bladder cancer tumours block the immune cells from accessing it by activating a cell signalling pathway called the peroxisome proliferator-activated receptor gamma (PPAR-γ) pathway.
“With this pathway, the tumours close the door to the immune system,” said Mads Daugaard, an Assistant Professor of urologic science at UBC ,”Without immune cells in the tumour, checkpoint immunotherapy has little effect. Now we know what door the tumours are closing and we can therefore focus our efforts on breaking down that door and let the immune system back in.”
The study finds that checkpoint immunotherapy, which is designed to activate the immune system, is not effective on some bladder cancers because there are no immune cells in the tumours. The finding explains what is happening at a cellular level to prevent the immune cells from getting into the tumour and points scientists in the right direction towards developing a combination therapy that could work.
“It’s been a mystery for decades as to how tumours escape the immune system,” said Prof Daugaard, “We’ve identified a cellular signalling pathway that regulates whether the body’s immune cells are allowed to infiltrate the tumour.”
Bladder cancer is the fifth most common cancer in Canada. There is only one line of chemotherapy available, cisplatin-based therapy, for invasive tumours. Once cancers become resistant, only checkpoint immunotherapy is approved as second-line treatment.
Atezolizumab is a checkpoint immunotherapy drug that strengthens the body’s immune response and recently became the first new bladder cancer drug to be approved in more than twenty years. Initial results were very promising but subsequent clinical trials have shown that only one in five patients showed an objective response to treatment. The reason for that has puzzled researchers, until now.
Prof Daugaard and his team have taken the first steps to develop a drug able to target the PPAR-γ pathway. The rationale is to use such a drug in combination with checkpoint immunotherapy treatment.
“The most efficient way to combat a cancer would be to have the immune system take care of it itself. This is ultimately what we want to achieve,” he said.
Related topics
Immuno-oncology, Immuno-oncology therapeutics, Oncology
Related conditions
Bladder cancer
Related organisations
H3 Biomedicine, The University of British Columbia
Related people
Assistant Professor Mads Daugaard, Dr Peter Black, Dr Ping Zhu