Researchers have developed a new bioreactor that can manufacture T cells faster than other technologies, which may advance immunotherapy.
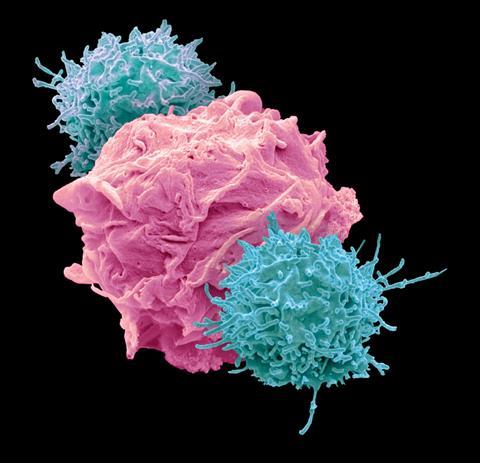
Immunotherapy, the promising therapy which harnesses the power of the body’s immune response to target cancer cells, may be advanced by a new minifridge bioreactor developed by researchers at Washington State University. This bioreactor can quickly manufacture T cells, cancer-killing white blood cells, at 95 percent of the maximum growth rate, which is 30 percent faster than other current technologies. The team used T cells from cattle, developed by co-author Bill Davis of WSU’s Veterinary College, and expect it will perform similarly on human cells.
There were over 1,400 different types of therapies using T cells, known as chimeric antigen receptor T cell (CAR-T) therapy in development in 2022. Seven of these were approved by the FDA for a variety of cancer treatments. However, the use of CAR-T cell therapy is limited due to the cost and time needed to grow T cells. Each infusion treatment for a cancer patient needs up to 250 million cells.
First author Dr Kitana Kaiphanliam, a postdoctoral researcher in WSU’s Gene and Linda Voiland School of Chemical Engineering and Bioengineering, said: “The manufacturing demand for this growing number of therapies is not being met, so there is a gap that needs to be filled in terms of biomanufacturing solutions.” She continued: “At the end of the day, they need to be upscaled, so they can be used by more people.”
Within the bioreactor, the growing cells are suspended as a dense cloud and are continuously bathed by an inward flow of medium containing nutrients, whilst being acted on by centrifugal force. Led by Chemical Engineering Dr Bernie Van Wie, Kaiphanliam’s advisor and a co-author on the paper, the prototype took four decades of research on designing a centrifugal bioreactor to rapidly densify and expand cells.
The most recent prototype is also self-contained within a sterile cabinet. Dr Kaiphanliam explained: “It acts like a biosafety cabinet. It can be used in circumstances where clean manufacturing facilities are not available or easily accessible, so it can democratise these cell-based therapies.”
To improve the bioreactor, the researchers aim to add multiple chambers and expect that they’ll eventually be able to produce enough cells in three days for three doses of a therapy. Also, they plan to start testing with human T cells and have begun communicating with cancer researchers on beta testing at the Fred Hutchinson Cancer Center. Dr Kaiphanliam and co-author Dr Brenden Fraser-Hevlin have begun Ananta Technologies Inc., with the hope to eventually produce and marketing the technology.
Dr Kaiphanliam said: “I recognised the potential that this bioreactor could have on cell-based therapies and manufacturing for these therapies, and I didn’t want to see it stuck in an academic laboratory." She continued: “I really hope having novel technologies to help with manufacturing reduces that financial barrier for these life-saving therapies.”
This work was published in Biotechnology Progress.