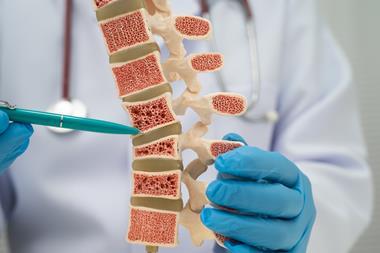
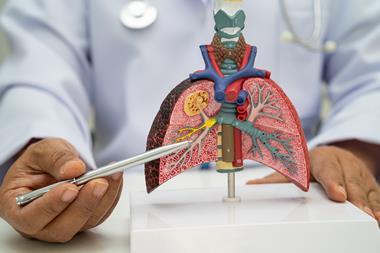
Treatment with Palbociclib and a compound targeting CAD increased survival to 100 percent for selected lymphoma cell lines.
Researchers at the Cleveland Clinic have identified an important mechanism used by Kaposi's sarcoma-associated herpesvirus (KSHV), also known as human herpesvirus 8 (HHV8), to induce cancer. The results suggest effective novel treatment options for KSHV-associated cancers, including Kaposi’s sarcoma (KS), HHV8-associated multicentric Castleman disease, and primary effusion lymphoma.
KSHV-induced cancers are aggressive and challenging to treat. The number of people with KSHV varies throughout the world, but an estimated 10 percent of people in North America and Northern Europe, and over 50 percent of individuals in parts of Northen Africa, are estimated to have it. However, these rates could be higher, as KSHV, like other herpesviruses, often goes undiagnosed due to a lack of symptoms. The virus remains dormant, suppressed by the immune system, but is reactivated when immunity is weakened, like in older people, those with HIV/AIDS, and transplant recipients. In these high-risk groups, the now active virus can trigger aggressive cancers.
Dr Jun Zhao, Cleveland Clinic Florida Research & Innovation Center, explained: “Our findings have significant implications: viruses cause between 10 percent to 20 percent of cancers worldwide, a number that is constantly increasing as new discoveries are made. Treating virus-induced cancers with standard cancer therapies can help shrink tumours that are already there, but it doesn’t fix the underlying problem of the virus.”
He continued: “Understanding how pathogens transform a healthy cell into a cancer cell uncovers exploitable vulnerabilities and allows us to make and repurpose existing drugs that can effectively treat virus-associated malignancies.”
CDK6 and CAD
Led by Dr Zhao, the team of researchers discovered that KSHV manipulates two human enzymes named CDK6 and CAD, which causes the infected cells to produce extra metabolites, thereby enabling faster replication of the virus and an uncontrolled proliferation of the cells.
The scientists treated preclinical models with Palbociclib, an FDA-approved breast cancer medication which blocks CDK6, as well as a compound targeting CAD, and observed significant decreases in tumour size and increases in cancer survival rates. Notably, most tumours virtually disappeared after around a month of treatment, remaining tumours shrank around 80 percent and survival increased to 100 percent for selected lymphoma cell lines.
The team are conducting further research into the connections between KSHV, CDK6/CAD pathway, and cancer formation. They hope to implement and refine their experimental drug combinations for clinical trials. Dr Zhao concluded: “By investigating these metabolic rewiring mechanisms, we aim to find the Achilles’ heel of cancer-causing viruses and non-viral cancers. I’m excited to see what the future of this work holds.”
This study was published in Nature Communications.