Anticancer drug as an alternative to liver transplant
Posted: 17 August 2018 | Drug Target Review | 1 comment
Mouse models showed promise when an anticancer drug was used to treat liver failure, resulting in liver regeneration and preventing liver related death…
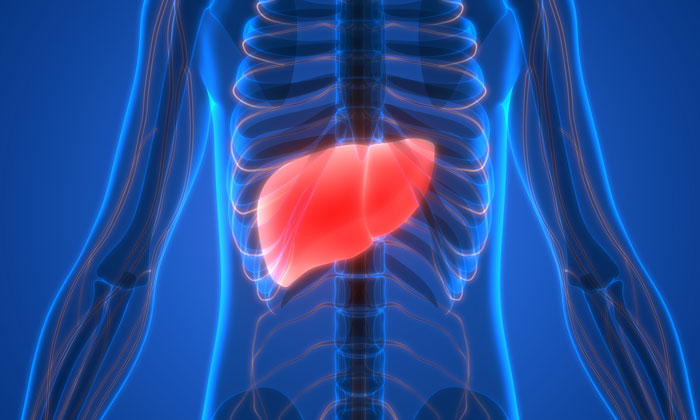

A recent study has identified that an anticancer drug could be used in place of a liver transplant when a patient suffers from sudden liver failure.
Researchers from the University of Edinburgh, and Cancer Research UK Beatson Institute in Glasgow found that liver injury in mice triggered a process called senescence, which is commonly associated with chronic disease or ageing.
Acute liver failure occurs when a healthy liver is seriously damaged and can no longer regrow and recover. This leaves patients in need of a liver transplant.
The liver helps to support other organs, processing digested food from the intestine, combating infection, detoxifying and removing harmful substances from the blood, manufacturing bile and hormones, and making enzymes and proteins responsible for many chemical reactions required by the body.
Damaged livers can often regrow and recover themselves, however when a large injury occurs, regeneration may fail. Even 24 hours without a fully working liver could be life threatening.
Many individuals end up with acute liver failure from paracetamol overdose, with around 200 UK and 2,000 US life threatening cases each year.
The researchers found that when anti-cancer drugs were used in mice with liver failure, the liver was able to regenerate, preventing death from liver injury.
Liver specialist and a Wellcome Trust Fellow, Dr Tom Bird said: “Through our research so far we have identified a potential treatment for acute liver failure, which may prevent the need for transplant. Most of the patients we see with this type of critical liver injury are otherwise physically healthy, and have accidentally or, often, sadly, intentionally taken an overdose of paracetamol.
“While transplant offers incredible life-saving opportunities for these patients, it does mean a major operation and a lifetime of medication and with around 300 adults and children in the UK in need of a liver transplant at any one time, it cannot be guaranteed.
“New treatments like this which set liver regeneration free and may prevent the need for liver transplants, would make a huge difference for these patients. They may also allow us to use the livers available for transplantation for other patients with different forms of liver disease who might otherwise die whilst waiting for a suitable liver donor.”
The team is hopeful that a therapy to prevent the need for a liver transplant may become available, following other investigations.
The study was published in Science Translational Medicine.
Related topics
Disease Research, Drug Discovery, Drug Targets, Research & Development, Therapeutics
Related conditions
liver failure
Related organisations
Cancer Research UK, Edinburgh University
Related people
Dr Tom Bird





all the information of this blog are very important anticancer data explain in this website one by one also drug and liver data also present we have also experience doctor Faisal dar in Pakistan.