Organoids grown from stem cells could treat children with intestinal failure
Posted: 8 September 2020 | Victoria Rees (Drug Target Review) | No comments yet
Intestinal organoids have been grown by researchers using stem cells from patient tissues that could lead to personalised transplants for children with intestinal failure.

Scientists report that they have grown human intestinal grafts, or organoids, using stem cells from patient tissue that could one day lead to personalised transplants for children with intestinal failure. The study was conducted at the Francis Crick Institute, Great Ormond Street Hospital (GOSH) and UCL Great Ormond Street Institute of Child Health (ICH), all UK.
Children with intestinal failure cannot absorb the nutrients that are essential for their overall health and development. In these cases, children can be fed intravenously, but this is associated with severe complications such as line infections and liver failure. If these complications arise, there is a shortage of suitable donor organs and problems can arise after surgery, such as the body rejecting the transplant.
In their proof-of-concept study, the research team showed how intestinal stem cells and small intestinal or colonic tissue taken from patients can be used to grow the important inner layer of small intestine in the laboratory with the capacity to digest and absorb peptides and digest sucrose in food.
“It is urgent that we find new ways to care for children without a working intestine because, as they grow older, complications from parental nutrition can arise,” said senior author Dr Vivian Li. “We have set out a process to grow one layer of intestine in the laboratory, moving us a step closer to being able to offer these patients a form of regenerative medicine, which uses materials created from their own tissue. This would reduce some of the risks that transplant patients face, such as their immune system attacking the transplant.”
The researchers took small biopsies of intestine from 12 children who either had intestinal failure or were at risk of developing the condition. In the lab, they then stimulated the biopsy cells to grow into “mini-guts”, or intestinal organoids, generating over 10 million intestinal stem cells from each patient over the course of four weeks.
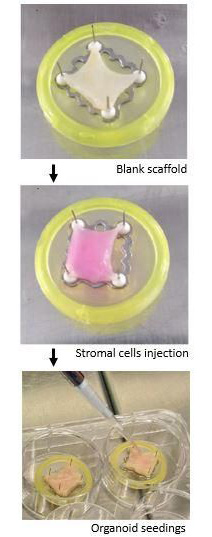

Credit: Francis Crick Institute.
The researchers also collected small intestine and colon tissue, that would otherwise have been discarded, from other children undergoing essential surgery to remove parts of their gut. Using laboratory techniques, cells were removed from these tissues leaving behind a skeleton structure which formed scaffolds.
The researchers placed the organoids onto these scaffolds, where they grew on this structure to form a living graft. Due to specific culture conditions, the stem cells changed into many of the different types of cells that exist in the small intestine. The grafts were able to digest and absorb peptides, the building blocks of proteins, as well as digest sucrose into glucose sugars.
“What is significant here is we have shown that scaffolds can be created using tissue from the colon, not only tissue from the small intestine. In practice, it is often easier to obtain tissue from the colon, so this could make the approach much more feasible. It is an important step forward in regenerative medicine and we are optimistic about what this means for patients, but more research lies ahead before we can safely and effectively translate this approach to treatment,” explained senior author Professor Paolo De Coppi, Consultant Paediatric Surgeon at GOSH and Head of Surgery, Stem Cells & Regenerative Medicine Section at the UCL Great Ormond Street ICH.
The researchers also demonstrated that the grafts survive and mature when transplanted into mice.
“By applying our basic science knowledge of intestinal stem cell biology, we have developed a time efficient and clinically relevant method for rebuilding human small intestine grafts for transplantation,” said lead author Laween Meran, Gastroenterology Registrar and Clinical Research Training Fellow at the Crick and the ICH. “Now that we have shown the grafts are successful on a small scale, the next crucial steps will be to start growing the other layers of the intestine such as muscle and blood vessels, whilst also scaling up our methods to create viable grafts relevant to individual patient needs”.
The study was published in Nature Medicine.
Related topics
Organoids, Personalised Medicine, Stem Cells
Related conditions
Intestinal failure
Related organisations
Francis Crick Institute, Great Ormond Street Hospital (GOSH), UCL Great Ormond Street Institute of Child Health (ICH)
Related people
Dr Vivian Li, Laween Meran, Professor Paolo De Coppi