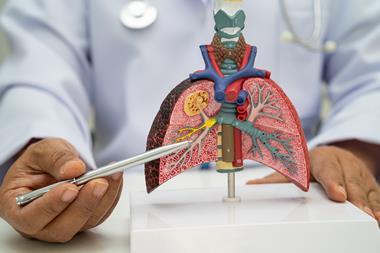
UW researchers at the Carbone Cancer Center have identified the cells that can cause graft versus host disease, the most common complication of bone marrow transplants.

A bone marrow transplant can be a lifesaving treatment for people with relapsed blood cancers, but a potentially lethal complication known as graft-versus-host disease put limitations on this procedure. New research from the University of Wisconsin–Madison, US, is helping to change that by identifying the cell population that causes graft-versus-host disease (GvHD), a target that may make bone marrow transplants safer and more effective. The study was recently published in Science Advances.
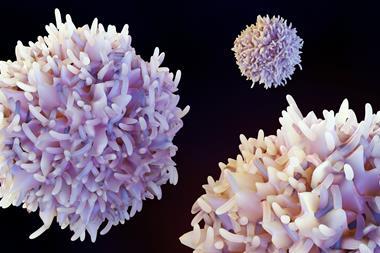
An allogenic bone marrow transplant is a common treatment for blood cancers and other diseases of the immune system. During the transplant, the patient’s immune cells are replaced with the donor’s healthy cells. While the donor cells can help cure the patient’s blood cancer, they can also cause GvHD — in which donor T cells, a specialised immune cell in the blood, attack the patient’s healthy cells. This causes complications similar to an autoimmune disease that can be lethal.
“GvHD is one of the most common complications after an allogeneic haematopoietic cell transplantation procedure, and the field knows quite well that the T cells from the donor are the ones mediating the disease,” said the study’s lead author Nicholas Hess. “Before this study, there was no finite T cell population that we have been able to identify as the cause of GvHD, so all our treatment regimens generally impacted the entire T cell population. But targeting all the T cells is not ideal, as they do not just cause this detrimental disease, they also have a beneficial impact on the ability to prevent relapses.”
The team identified cells called CD4/CD8 double positive T cells (DPT) causing GvHD in immunodeficient mice. To further confirm their findings, the researchers directly investigated human patient samples.
“We looked at over 400 clinical samples from 35 patients as a part of this study and found double positive T cells to be predictive of GvHD. We also found four other biomarkers which are predictive of not just GvHD, but also relapse in general,” said Hess. “Based on that, our next step is to merge the biomarkers into a machine learning algorithm that can output a risk prediction model. Clinicians could then use this model to understand a patient’s risk of relapse and GvHD.”
A team of physicians and scientists at UW–Madison is working on ways to address the problematic cells in patients while leaving healthy and helpful T cells to flourish. Hess says that while the team is very confident the double positive T cells are directly involved in GvHD, the key step in bringing this discovery to the clinic will be developing a targeted depletion strategy and this prediction model.
“When we can gain confidence in this biomarker research and our ability to identify patients at risk, then we will potentially be able to treat them before they have all the detrimental effects of this disease,” Hess concluded.