A new study has identified targets to refine diagnostic tests, track disease progression, and discover more effective therapies.
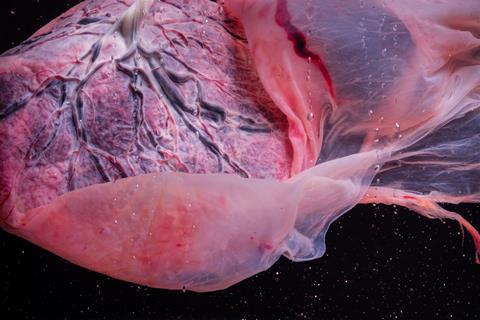
Researchers at the University of California Los Angeles (UCLA) have conducted a study which could change the way scientists understand, diagnose and treat placenta accreta spectrum (PAS) disorder. This disorder is a serious condition in which the placenta, the temporary organ that provides support for a foetus, fails to separate from the uterus at birth, risking the health, and potentially the life, of both mother and baby. In recent decades, the incidence of PAS disorders has increased. Although the cause of this is unknown, caesarean deliveries is one of the risk factors.
Previously, scientists believed that trophoblasts, overly invasive placental cells, were responsible for keeping the connection intact. However, the new study identifies genetic and cellular changes within single cells where the placenta and uterus join, which alters the focus to how the structural support of tissues, and the blood vessels of the uterus, are significant.
Dr Yalda Afshar, a maternal-foetal medicine specialist and researcher at the David Geffen School of Medicine at UCLA, explained: “We utilised two new techniques in single-cell analysis to create an atlas of cells involved in placenta accreta to better understand this increasingly prevalent disorder that can have devastating implications for maternal and neonatal health.”
The paper’s senior author, Dr Deborah Krakow, added: “This work revealed a subset of genes differentially expressed in placenta accreta spectrum disorder, which provides the basis for the ‘permissive environment’ for the placenta to attach to the uterine lining.” Dr Krakow is a maternal-foetal medicine specialist and researcher and chair of the Department of Obstetrics and Gynaecology at the David Geffen School of Medicine at UCLA.
The research demonstrated that when a pregnant person has a placenta accreta, the decidua, the layer of the uterine lining that forms during pregnancy, and blood vessels, are sending different signals to the placenta. Normally, the placenta is shed after birth, but in placenta accreta, it is stuck on too tight, which is a reason for multiple maternal complications.
The team performed multiple placental biopsies on 12 placentas: six controls and six placentas with PAS disorder. They then conducted single-cell RNA analysis on 31,406 individual cells, and also applied spatial transcriptomics to 36 regions of interest: 12 in PAS-adherent, 12 in PAS-nonadherent, and 12 in controls.
“Our goal was to characterise the intimate relationship between the maternal and foetal tissue at the site of accreta or malfunction,” Dr Afshar stated. “The genes and signalling pathways we identified go beyond providing a better understanding of the mechanism of the disease; they may be used as targets to help us refine diagnostic tests, track disease progression over time, and discover new, more effective therapies.”
This study was published in the American Journal of Obstetrics & Gynaecology.