A living material resembling sputum from CF patients can grow biofilms, enabling scientists to assess the effectiveness of antimicrobials.
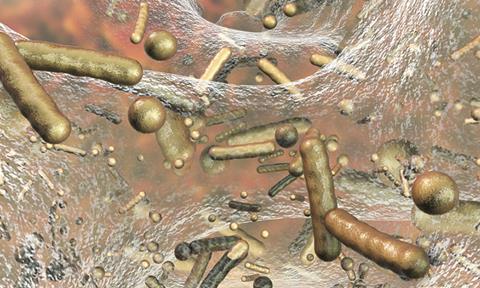
A living material resembling human phlegm has been engineered by scientists from the University of Nottingham, which will enable them to gain a better understanding of how a specific infection develops on the lungs of people with cystic fibrosis (CF).
Led by Dr Yuanhao Wu, the study was also a collaboration between Dr Alvaro Mata from the School of Pharmacy and Department of Chemical Engineering and Dr Miguel Cámara from the National Biofilms Innovation Centre in the School of Life Sciences at the University of Nottingham.
Biofilms are strong living three dimensional (3D) materials that have essential functions in nature, but also cause major problems, like the contamination of hospital surfaces, or in our antibiotic treatment tolerance. The lack of biofilm models is one of the largest challenges in antimicrobial discovery, as they need to demonstrate the complexity of natural environments, such as those encountered in the lung of CF patients. These patients have a genetic alteration which means they are unable to clear infections in their lungs. Communities of disease-causing microbes accumulate within thick mucus forming 3D biofilms. These biofilms are highly resistant to antibiotics so there is a significant need to develop in vitro models which can reliably reproduce them in the lab.
These models will provide more consistent evaluations of new therapeutic actions before being taking into pre-clinical studies and will be crucial for answering fundamental research questions on the interactions polymicrobial biofilms and their host which lead to chronic infections.
Engineering phlegm
The researchers engineered a living material resembling natural sputum (phlegm) from CF patients that can grow 3D polymicrobial biofilms in a controlled manner, resembling those found in the CF lung. The team achieved this by combining peptides with a culture medium that is known to recreate natural sputum and can be infected easily.
“The capacity to create complex 3D biofilms in the lab in a simple manner, will lead to practical tools to better understand how these living structures form and how to treat them better.”
The living material has multiple microbial communities and key nutritional and chemical factors that promote bacterial growth and exhibit physical properties mimicking those of CF sputum biofilms. The material has been used to build an infected in vitro lung epithelial model that was used to investigate the impact of antibiotics.
Dr Mata says: “The capacity to create complex 3D biofilms in the lab in a simple manner, will lead to practical tools to better understand how these living structures form and how to treat them better.”
Dr Cámara says: “The technology developed in this study will revolutionise the way we study biofilm-mediated infections and assess the effectiveness of novel antimicrobials using different in vivo-like infection environments.”
The study was published in Matter.