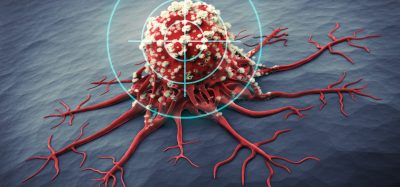
“Blood vessel growth is critical to tumour growth,” said Dr John Lewis, the Alberta Cancer Foundation Frank and Carla Sojonky Chair in Prostate Cancer Research at the University of Alberta. “When a tumour starts growing, cells start to divide out of control and they lack an organised blood vessel network to feed them. When that happens, there are help signals that tell the surrounding blood vessels to branch off and supply a tumour with new blood vessels for oxygen and nutrients.”
There are a number of approved cancer drugs to prevent the formation of a new tumour related blood vessels, but according to Dr Lewis, many haven’t yet lived up to their promise due to wide variability among patients.
An imaging agent could be used before treatment to see how many new blood vessels are forming.
He believes the newly created imaging agents, which can be used in PET scans and fluorescence imaging, could provide doctors helpful insight when determining the best course of action for their patients.
“These drugs can be toxic and expensive, but potentially life-saving for certain patients. An imaging agent could be used before treatment to see how many new blood vessels are forming to determine whether an individual patient is a candidate for treatments that will inhibit new blood vessel growth.’ This would allow treatment to be personalised for those patients most likely to respond. Also, during the treatment, you could use the same imaging agent to monitor the response to the therapy.”
In his research, Dr Lewis, along with collaborators at Western University and Case Western Reserve University, worked with a protein, EGFL7, that is specific to actively growing blood vessels. Together they created new peptides that home into EGFL7 to test if they would be useful for imaging purposes.
“Once we had the peptide, we validated in two ways,” said Dr Lewis. “First we did some PET imaging of mice tumours and the peptide localised to those tumours and lit them up. We also created nanoparticles with the peptide and they were able to accumulate in the new blood vessels and light them up as well.”
The imaging agents now need to be tested in a treatment setting. Dr Lewis plans to begin that work in animal models before moving on to clinical work in humans. His aim is to provide new tools which will help doctors make better and quicker treatment decisions for their patients.
“Ideally we would get a measure of response 24 hours after we first give the drug,” said Dr Lewis, “Currently we measure any changes in tumour size up to a month after treatment, which is a long time to wait to find out if an expensive drug isn’t working.”