Urine tests are important in diagnosing myeloma
Posted: 16 July 2018 | Drug Target Review | No comments yet
It may be better to examine the urine and the blood of patients suspected of tumours of the plasma cells…
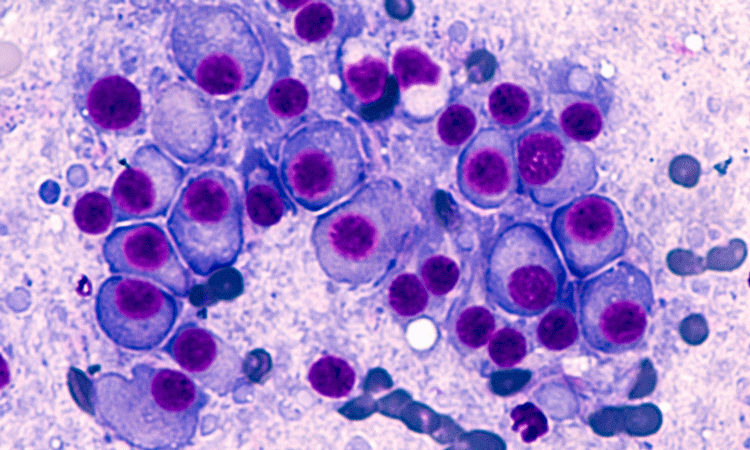

Researchers found that it may be more beneficial testing the urine and the blood of suspected cases of multiple myeloma, to prevent the false negatives that occur 25 percent of the time. The condition, monoclonal gammopathy, is one in which plasma cells begin to make one immunoglobin (antibody), in place of a vast collection of antibodies. The result of this can be the cancer multiple myeloma.
Originally, the urine test was used by physicians and pathologists, but its use declined when the serum free light chain assay became available approximately 12 years ago. As such, some physicians believe the urine test to be redundant.
These tests check for signs of the abnormal antibody, and check the serum or urine for light chains, an abnormality in the usual ratio between two types of a portion of the antibody.
Dr Gurmukh Singh, vice chair of clinical affairs for the Department of Pathology at the Medical College of Georgia (MCG) at Augusta University (AU), said “When you test the serum, we suggest you also test the urine whenever you suspect that somebody has a tumour of the plasma cells.”
The study reviewed 175 patients, with serum protein electrophoresis/serum protein immunofixation electrophoresis; urine protein electrophoresis/urine protein immunofixation electrophoresis and serum free light chain assays from 2010 to 2016. The team identified that if the multiple myeloma is linked with the lambda light chain, there is a 25 percent chance it will not be detected by the serum test for free light chains.
“If you have a lambda chain-associated lesion and you don’t do a urine study, [and] just rely on the serum free light chain assay, about 1 out of 4 times, the assay will tell you that you don’t have anything when you actually do,” says Dr Won Sok Lee, co-author and fourth-year pathology resident at MCG and AU Health.
Immune cells in bone marrow are called plasma cells, and produce immunoglobins; antibodies that attach to, and destroy invading cells. When plasma cells do not work as they should, they begin to produce a single, dysfunctional immunoglobin.
This y-shaped immunoglobin is comprised of pieces of protein called ‘light’ and ‘heavy’ chains. Light chains have two different types, kappa and lambda, each distinctive in its amino acid sequence. Cancer can affect both types of light chain.
Dr Singh stated that in multiple myeloma, the relevant chain production increases, however kappa increases far more. Occasionally, the ratio is normal, despite an abnormal lambda immunoglobin showing up in the urine.
The researchers describe how nearly 40 percent of patients have an abnormal ratio without having monoclonal gammopathy.
Dr Lee describes how these variabilities mean that some patients may go undiagnosed; particularly those with less-common lambda chain associated lesions.
“You may go undiagnosed because the serum free light chain test either is not picking up those abnormal proteins or the lambda lesions don’t make that many excess abnormal proteins,” Singh notes.
The false negatives described may be accounted for by the underdetection of lambda light chains in serum, especially since this abnormal antibody produced by a lambda lesion was highlighted in the urine test. The researchers also stated that underproduction of the lambda free light chains in these patients likely account for another 5 percent of false negatives.
The ratio of kappa to lambda depicted excess kappa chains in approximately 90 percent of patients who had an abnormal ratio, without a tumour of the plasma cells.
The team found that there is a high false negative rate for a lambda-dominant ratio in monoclonal gammopathies associated with lambda chains, presumably due to the underdetection of lambda light chains in the serum.
Here lies the problem with not aiming to identify errant antibodies and light chain ratios in urine, said Dr Lee. While ratios can seem normal in the serum, urine has monoclonal lambda chains.
“If it’s in the urine, you are making abnormal free light chains,” stated Dr Lee. Equally, the ratio can look normal in the serum in people who do not have cancer.
Despite it being more expensive, the urine test seems a better diagnostic tool in this case, since it enables the pathologist to give more detailed results to physicians, and in turn, patients.
Using the serum free light chain assay, the researchers found a systematic underdetection of serum free lambda light chains, along with an underdetection of the lambda dominant ratio.
Examining the serum free light chains is recommended for diagnosing and monitoring monoclonal gammopathies, and although there are varying opinions on its usefulness, if initial tests indicate a problem, a bone marrow biopsy is performed to confirm the diagnosis.
Excessive light chains produced ordinarily are easily excreted in the urine because of their small size. With monoclonal gammopathy, some of these can get trapped in the kidneys, damaging their function.
The study was published in the Journal of Clinical Medicine Research.
Related topics
Analytical Techniques, Assays, Disease Research
Related conditions
Cancer, multiple myeloma
Related organisations
Augusta University
Related people
Dr Gurmukh Singh, Dr Won Sok Lee