COVID vaccine that could protect against Omicron and other variants
Posted: 14 April 2022 | Ria Kakkad (Drug Target Review) | No comments yet
The antigen-based vaccine has the potential to induce sterilising immunity to old and new SARS-CoV-2 variants by preventing infection by stopping viral replication and transmission through the inhibition of cellular virus entry.

The preclinical data for a vaccine developed at MedUni Vienna, Austria to protect against SARS-CoV-2 indicates that it is effective against all SARS-CoV-2 variants known to date, including Omicron. The antigen-based vaccine has the potential to induce sterilising immunity to old and new SARS-CoV-2 variants by preventing infection by stopping viral replication and transmission through the inhibition of cellular virus entry. The vaccine could also protect those who have not yet built up any immunity as a result of vaccination as they will receive additional T-cell support from the PreS portion of the vaccine. The data from the study were recently published in the leading journal Allergy.
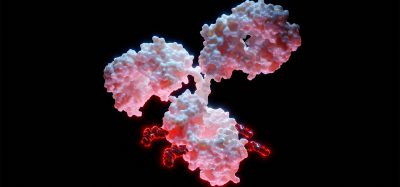
The antigen-based targets the receptor binding domains (RBD) of the SARS-CoV-2 virus and induced a robust and uniform RBD-specific IgG antibody response in animal models and in human tests. This antibody response prevents the virus from docking onto and entering the body’s cells, so that infection cannot occur.
The SARS-CoV-2 subunit vaccine (PreS-RBD) developed at MedUni Vienna is based on a structurally folded fusion protein consisting of two receptor binding domains (RBD) of the SARS-CoV-2 virus and the PreS antigen from hepatitis B, which serve as immunological carriers for each other, thereby strengthening the immune response. Currently available genetic SARS-CoV-2 vaccines induce mainly transient IgG1 antibody responses, whereas the PreS-RBD vaccine can additionally induce long-lived RBD-specific IgG4 antibodies.
PreS-RBD-specific IgG antibodies detected in blood and mucosal secretions reacted with SARS-CoV-2 variants, including the Omicron variant. Antibodies induced by vaccination with PreS-RBD more potently inhibited the binding of RBD with its human receptor ACE2, and their virus-neutralising titers were higher than those in a random sample of individuals fully immuniSed with two vaccinations of currently registered vaccines or than those of COVID-19 convalescents.
The development of this Austrian COVID vaccine was to a large extent inspired by decades of experience in allergy vaccine design. Previous work on allergy vaccines and clinical trials also conducted with PreS-based allergy vaccines have demonstrated the safety of PreS-based vaccines, even when used repeatedly.
“Our data give us grounds to hope that this readily producible protein-based vaccine antigen will be effective against all SARS-CoV-2 variants known to date, including omicron,” said study leader Rudolf Valenta. “The vaccine is designed to enable repeated injections to build up sustained sterilizing immunity, is suitable for use in all age and risk groups and appears to be superior to currently available vaccines when it comes to inducing neutralising antibodies.”
If sufficient funding is forthcoming, the first clinical trials required for approval could be carried out this year.
Related topics
Antibodies, Research & Development, Targets, Vaccine
Related conditions
Covid-19
Related organisations
MedUni Vienna
Related people
Rudolf Valenta