Progress towards a stem cell-based therapy for blindness
Posted: 1 August 2022 | Ria Kakkad (Drug Target Review) | No comments yet
Scientists are developing an effective stem cell-based therapy to regenerate photoreceptors cells and restore sight in people with blindness.


Researchers at the University of Pennsylvania, US have made significant progressed towards a cell-based therapy to treat blindness. Previous treatments met with several challenges, including introduced cells dying rapidly or failing to integrate with the retina. However, in their new study, which was recently published in Stem Cell Reports, the researchers introduced precursors of human photoreceptor cells into the retinas of dogs. A cocktail of immunosuppressive drugs enabled the cells to survive in the recipients’ retinas for months, where they began forming connections with existing retinal cells.
The researchers have been interested in addressing retinal blinding disorders and they have had great successes to date at producing corrective gene therapies for conditions with known causative genes. But for many cases of inherited retinal degeneration, a gene has not been identified. In other patients, the disease has progressed so far that no photoreceptor cells remain intact enough for gene therapy. In either scenario, a regenerative medicine approach, in which photoreceptors could be regrown outright, would be extremely valuable.
Photoreceptor cells, which are made up of rods and cones, constitute a layer of the outer retina critical to initiating the process of vision, whereby the energy of light transforms into an electrical signal. To function properly, they must form a connection, or synapse, with cells of the inner retina to pass along the visual information. Thus, the goal of this cell therapy is to recreate this layer and enable it to integrate with the retina’s other cell types to relay signals from one layer to the next.
In the current work, the team used stem cell–derived precursors of human photoreceptor cells developed in the lab to serve as the basis of the cell therapy. The researchers developed a new surgical approach to inject the cells, which were labelled with fluorescent markers, into the retinas of seven dogs with normal vision and three with a form of inherited retinal degeneration, then used a variety of non-invasive imaging techniques to track the cells over time.
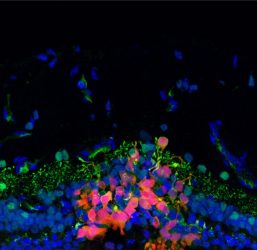

Following a transplantation procedure, human photoreceptor precursor cells labelled red migrated and integrated into a degenerated canine retina. The green label is a synaptic maker, suggesting the transplanted cells began forming a connection with second-order neurons in the retina
[Credit: Courtesy of the Beltran lab/Stem Cell Reports].
The researchers observed that cell uptake was significantly better in the animals with retinal degeneration compared to those with normal retinas.
“What we showed was that, if you inject the cells into a normal retina that has its own photoreceptor cells, the retina is pretty much intact and serves as a physical barrier, so the introduced cells do not connect with the second-order neurons in the retina, the bipolar cells,” said Professor William Beltran. “But in three dogs that were at an advanced stage of retinal degeneration, the retinal barrier was more permeable. In that environment, cells had a better ability to start moving into the correct layer of the retina.”
Because the transplanted human cells could be interpreted by the dogs’ immune system as foreign entities, the researchers did what would be done in other tissue transplant procedures: They gave the dogs immunosuppressive drugs.
Indeed, while the injected cell populations declined substantially in dogs that did not receive the immune-suppressing drugs, the cell numbers dipped but then sustained in the dogs that received the cocktail.
The next stage for this project will be to continue optimising the therapy, and then test whether there is a functional response—in other words, improved vision—in its recipients.
Related topics
Cell Therapy, Disease Research, Gene Testing, Regenerative Medicine, Therapeutics
Related conditions
blindness
Related organisations
Pennsylvania University
Related people
Professor William Beltran