New discovery could lead to treatment for cardiac hypertrophy
Posted: 15 June 2022 | Ria Kakkad (Drug Target Review) | No comments yet
Scientists have identified an important new mechanism that causes the heart’s muscle to thicken which markedly increases the risk of irregular heart rhythms and cardiac hypertrophy.
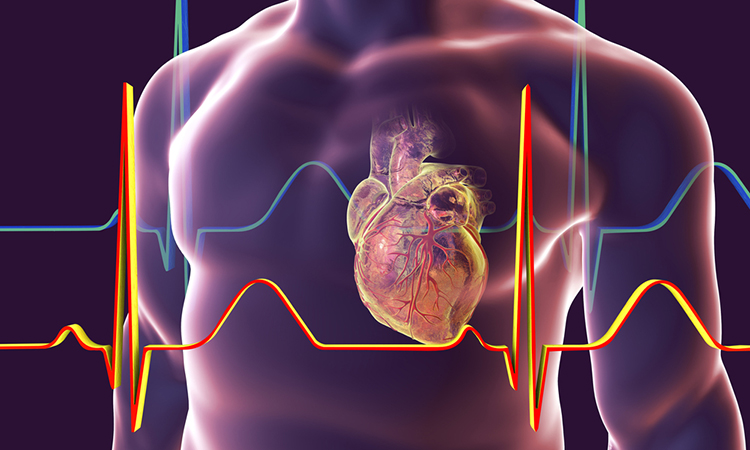
A new study has revealed an important new mechanism that causes the heart’s muscle to thicken which markedly increases the risk of irregular heart rhythms and heart failure. The discovery by a team at the Victor Chang Cardiac Research Institute, Australia, could herald the way for a new treatment for the heart disorder known as cardiac hypertrophy. The ground-breaking results were recently published in Nature Cardiovascular.
“Cardiac hypertrophy is a key risk factor for premature cardiac death and is a major cause of heart failure,” said Professor Brois Martinac, the lead author of the paper. “We have finally been able to pinpoint one of the key reasons why the heart muscle wall thickens and identified the molecules and the pathways that cause this process to take place.”
Cardiac hypertrophy is caused by many common conditions including abnormally high blood pressure and narrowing of one of the heart valves, aortic stenosis. It is a condition that causes the wall of the main pumping chamber, left ventricle, to thicken. Over time this thickening can cause abnormal heart rhythms and lead to heart failure. Once heart failure develops, the five-year survival is less than 50 percent.
The new research identified the exact molecules in the heart muscle cells responsible and crucially discovered how they were communicating with one another in a mouse model. They discovered that a molecule called Piezo1 triggered a signalling process, with another partner molecule, in cardiac muscle cells.
The discovery paves the way to develop a peptide that will stop these molecules from ‘talking’ to each other. This could prevent the heart muscle from thickening in the first place or stop any further thickening in those already affected.
Currently, there are few therapeutic options for severe hypertrophy. The traditional approaches include lowering the patients’ blood pressure or replacing a stenotic aortic valve – neither of which can reverse the damage caused by hypertrophy.
Fellow author Dr Jane Yu said: “We hope that in the long-term, as soon as we see evidence of heart muscle thickening you will be given a treatment, perhaps a small peptide, that will stop the process from progressing in your heart. This could even potentially be given to people with severe hypertension to avoid them developing cardiac hypertrophy in the first place. This preventative treatment could make a huge inroad into reducing the number of people affected by heart disease in Australia and save many lives in the future.”
The same team at the Institute is also exploring how this discovery could also help with the recovery of heart attack victims.
“When someone has a heart attack, many of their muscle cells will die and the heart loses its ability to pump as effectively, so it will compensate by thickening its muscle wall. A therapeutic that halted this process could be transformative for people who have a heart attack and prevent deaths in the longer-term post-heart attack”, concluded Martinac. “Whilst this is early days in our research, there are similar treatments showing promise in stroke victims, so we are incredibly excited about the potential of our discovery.”
Related topics
Disease Research, Molecular Biology, Molecular Targets, Peptide Therapeutics
Related conditions
cardiac hypertrophy
Related organisations
Victor Chang Cardiac Research Institute
Related people
Dr Jane Yu, Professor Brois Martinac