Ground-breaking 3D bioprinted tumours aid immunotherapy research
Posted: 20 October 2022 | Izzy Wood (Drug Target Review) | No comments yet
A team of scientists have 3D bioprinted breast cancer tumours and treated them in a new study, offering greater understanding of the disease.
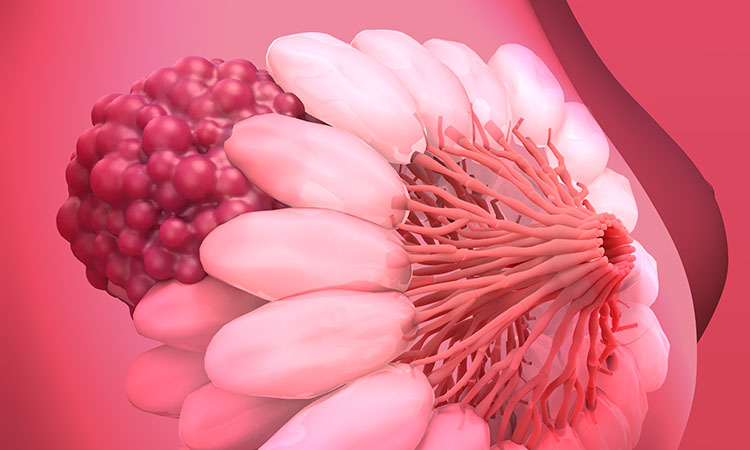

Researchers at Penn State, US have successfully three-dimensionally (3D) bioprinted breast cancer tumours and treated them in a breakthrough study to better understand the disease that is one of the leading causes of mortality worldwide.
Professor Ibrahim Ozbolat, senior author of the study, specialises in 3D printing to create tissues for use in human health. Two journal articles about the lab’s work using 3D bioprinting to help in the study of breast cancer were recently published in Advanced Functional Materials and Biofabrication.
The researchers used the relatively new technique called aspiration-assisted bioprinting to precisely locate tumours in 3D and create the tissue. They then formed the tissue into a multi-scale vascularised breast tumour model with blood vessels. The model responded to chemotherapy and cell-based immunotherapeutics.
The team validated the accuracy of the tumour model by treating it with doxorubicin, an anthracycline-based chemotherapeutic drug. Finding that the bioprinted tumour responded to chemotherapy, they then tested a cell-based immunotherapeutic treatment on the tumour.
Human CAR T cells were engineered via gene editing to recognise and fight an aggressive form of breast cancer. After 72 hours of circulating the edited CAR T cells through the tumour, the researchers found that the cellshad generated a positive immune response.
“Our model is made from human cells, but what we make is a very simplified version of the human body,” Ozbolat said. “We are aiming for simplicity within complexity. We want to have a fundamental understanding of how these systems work — and we need the growth process to be streamlined, because we do not have time to wait for tumours to grow at their natural pace.”
Ozbolat explained that despite remarkable advances in cancer treatment, there are a lack of pre-clinical platforms for studying experimental anticancer agents. Having to rely on clinical trials to test the efficacy of treatments limits the successful clinical translation of anticancer therapeutics.
Thus, the development of bioprinted models propose entirely new ways of understanding the tumour microenvironment and the body’s immune response.
“Immunotherapy has already been shown to be a promising treatment for haematologic malignancies,” Ozbolat said. “Essentially, immune cells of the patient are removed and gene-edited to be cytotoxic for cancer cells, then reintroduced into the patient’s bloodstream. Circulation is critical because the altered cells need to move around the body. With tumours, that kind of effective circulation does not exist, so we built our model to try to better understand how tumours respond to immunotherapy.”
Ozbolat and his colleagues are now working with tumours removed from actual breast cancer patients. The researchers will apply immunotherapeutics to patient-derived tumours to see how they respond.
“This is an important step in understanding the intricacies of the disease, which is essential if we are going to develop novel therapeutics and targeted therapies against cancer,” Ozbolat added.
A scientific first, the achievement lays the foundation for precision fabrication of tumour models. The advancement will enable future study and development of anti-cancer therapies without the use of in vivo experimentation.
“This will help us understand how human immune cells interact with solid tumours,” commented Ozbolat. “We have developed a tool that serves as a clinical test platform to safety and accurately evaluate experimental therapies. It is also a research platform for immunologists and biologists to understand how the tumour grows, how it interacts with human cells and how it metastasises and spreads in the body.”
Related topics
Bioengineering, Bioprinting, Cell Regeneration, Chimeric Antigen Receptors (CARs), Drug Targets, Organoids, Structural Biology, Therapeutics
Related conditions
Breast cancer
Related organisations
Penn State
Related people
Professor Ibrahim Ozbolat