Stem cell study reveals how neurons from PTSD patients react to stress
Posted: 24 October 2022 | Ria Kakkad (Drug Target Review) | No comments yet
The findings provide insight into how genetics can make someone more susceptible to developing PTSD following trauma exposure.

Stem cell-derived neurons from combat veterans with post-traumatic stress disorder (PTSD) react differently to a stress hormone than those from veterans without PTSD, a finding that could provide insights into how genetics can make someone more susceptible to developing PTSD following trauma exposure.
The study, published in Nature Neuroscience, is the first to use induced pluripotent stem cell (iPSC) models to study PTSD. It was conducted by a team of scientists from the Icahn School of Medicine at Mount Sinai, the James J. Peters Veterans Affairs Medical Center, the Yale School of Medicine and The New York Stem Cell Foundation Research Institute (NYSCF), all US.
Post-traumatic stress disorder can develop following severe trauma and is an enormous public health problem for both veterans and civilians. However, the extent to which genetic and environmental factors contribute to individual clinical outcomes remains unknown. To bridge this information gap, the research team studied a cohort of 39 combat veterans with and without PTSD who were recruited from the James J Peters Veterans Affairs Medical Center. Veterans underwent skin biopsies and their skin cells were reprogrammed into iPSC.
“Reprogramming cells into iPSC is like virtually taking cells back in time to when they were embryonic and had the ability to generate all the cells of the body,” said Dr Rachel Yehuda, senior author of the paper. “These cells can then be differentiated into neurons with the same properties as that person’s brain cells had before trauma occurred to change the way they function. The gene expression networks from these neurons reflect early gene activity resulting from genetic and very early developmental contributions, so they are a reflection of the ‘pre-combat’ or ‘pre-trauma’ gene expression state.”
To mimic the stress response that triggers PTSD, the scientists exposed the iPSC-derived neurons to the stress hormone hydrocortisone, a synthetic version of the body’s own cortisol that is used as part of the “fight-or-flight” response.
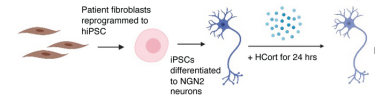
Graphic representation: skin cells being reprogrammed into induced pluripotent stem cells, then into neurons that were exposed to stress hormone and subsequently observed by the study team
[Credit: Yale School of Medicine].
“The addition of stress hormones to these cells simulates biological effects of combat, which allows us to determine how different gene networks mobilise in response to stress exposure in brain cells,” explained Yehuda.
Using gene expression profiling and imaging, the scientists found that neurons from individuals with PTSD were hypersensitive to this pharmacological trigger. The scientists also were able to identify the specific gene networks that responded differently following exposure to the stress hormones.
The team’s gene expression analysis revealed a set of genes that were particularly active in PTSD-prone neurons following their exposure to stress hormones.
“Importantly, the gene signature we found in the neurons was also apparent in brain samples from deceased individuals with PTSD, which tells us that stem cell models are providing a pretty accurate reflection of what happens in the brains of living patients,” noted Dr Daniel Paull, who co-led the study.
Moreover, the distinctions between how PTSD and non-PTSD cells responded to stress could be informative in predicting which individuals are at higher risk for PTSD.
“What is really exciting about our findings is the opportunities they offer for accelerating the diagnosis and treatment of PTSD,” Paull continued. “Importantly, having a robust stem cell model provides an ideal avenue to drug screening ‘in the dish,’ even across diverse patient populations.”
The researchers plan to continue leveraging their iPSC models to further investigate the genetic risk factors pinpointed by this study and to study how PTSD affects other types of brain cells, helping to broaden opportunities for therapeutic discovery.
Related topics
Genetic Analysis, Induced Pluripotent Stem Cells (iPSCs), Neurons
Related conditions
Post-traumatic stress disorder (PTSD)
Related organisations
Icahn School of Medicine at Mount Sinai., James J. Peters Veterans Affairs Medical Center, New York Stem Cell Foundation Research Institute (NYSCF), the Yale School of Medicine
Related people
Dr Daniel Paull, Dr Rachel Yehuda