Study reveals novel targets for treating atopic dermatitis
Posted: 12 January 2021 | Hannah Balfour (Drug Target Review) | No comments yet
Understanding how Staphylococcus aureus bacteria colonises skin affected by atopic dermatitis could lead to new treatments that help prevent the spread of antibiotic resistance, say scientists.
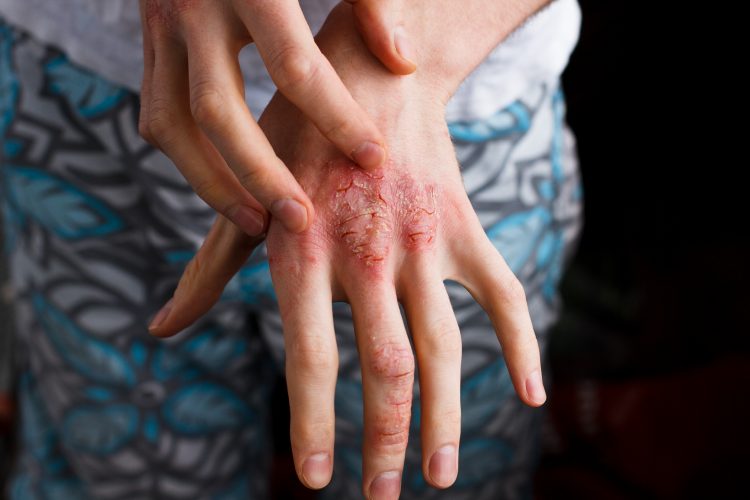

Researchers have uncovered a key mechanism underlying bacterial skin colonisation in atopic dermatitis. The scientists suggest their discovery could result in novel therapeutic options for treating Staphylococcus aureus infections, which are especially important as the prevalence of antibiotic resistant strains, like methicillin-resistant Staphylococcus aureus (MRSA), continues to rise.
Atopic dermatitis (AD), also called eczema, is the most common chronic inflammatory skin disorder in children, affecting between 15 and 20 percent. During disease flares, patients experience painful inflamed skin lesions accompanied by intense itch and recurrent skin infections.
S. aureus is a bacterium which colonises skin affected by AD, by doing so, it increases inflammation and exacerbates the symptoms of the disorder. Although a small number of therapies are available for patients with moderate to severe AD, researchers believe it is vital that we understand how S. aureus colonises AD skin so that new treatments directly targeting the bacterium can be developed.
To identify the human and bacterial factors that enable S. aureus to interact with AD skin, researchers from Trinity College Dublin’s School of Genetics and Microbiology and School of Clinical Medicine studied the attachment of the bacterium to corneocytes – the flattened, dead skin cells which comprise the outermost layer of the skin.
In their study, the team found that S. aureus binds to a specific region of a protein, called corneodesmosin, located on the surface of AD patient corneocytes. The importance of this interaction was highlighted when the scientists showed that bacterial binding to corneocytes could be reduced in vitro if the relevant region of corneodesmosin is blocked with an antibody.
In lab experiments, Dr Aisling Towell, a PhD graduate in Microbiology at Trinity, showed that bacterial interaction with corneodesmosin relies on two proteins attached to the surface of S. aureus: FnBPB and ClfB.
Dr Joan Geoghegan, Associate Professor of Microbiology in Trinity’s Department of Microbiology, explained why the results were significant: “Our findings provide new insights into how S. aureus bacteria attach to corneocytes at the skin surface, which is a crucial step during colonisation. Specifically, our discovery of an interaction between bacterial proteins and corneodesmosin on AD patient corneocytes is a key advance that could pave the way towards developing targeted approaches for preventing S. aureus skin colonisation in AD.”
Alan Irvine, Professor of Dermatology at Trinity, added: “AD is both a common and incredibly uncomfortable condition that has a massive impact on quality of life in both children and adults. Colonisation of the skin with S. aureus is a major driver of AD and a cause of disease flares. By identifying a major mechanism through which S aureus binds to the skin of patients with AD we have opened the possibility of targeting this pathway as a therapeutic option in AD.
“Targeting S. aureus binding to human skin by using small molecules would be a welcome addition to our therapeutic options. This is especially important in an era where antimicrobial resistance is an emerging global threat.”
The study was published in Proceedings of the National Academy of Sciences.
Related topics
Cell-based assays, Disease Research, Drug Development, In Vitro, Protein, Therapeutics
Related conditions
Atopic Dermatitis, methicillin-resistant Staphylococcus aureus (MRSA), Staphylococcus aureus
Related organisations
Trinity College Dublin
Related people
Alan Irvine, Dr Aisling Towell, Dr Joan Geoghegan