Identification of hits and leads for human African trypanosomiasis
Posted: 13 December 2017 | Dr Sheraz Gul, Giulia Pasini, Maria Paola Costi | No comments yet
Neglected tropical diseases (NTD) affect more than one billion people and new targets and drugs are needed to tackle these infections. The multi-disciplinary NMTrypI consortium has identified a number of different compound classes which could be effective against these diseases. This article reviews some of these compounds…


According to the World Health Organization, neglected tropical diseases (NTD) are a diverse group of communicable diseases that are prevalent in many tropical and sub-tropical regions and affect more than one billion people. These regions are associated with poverty and lack of suitable sanitation, and their populations are in close contact with infectious vectors. The situation is further confounded by the lack of new drugs being developed to treat these diseases.
In order to address this, the European Union in its Drug Development for Neglected Diseases Initiative has invested significantly towards research activities to discover new drugs for NTD. The funded consortia focus on epigenetic (A-PARADDISE), phosphodiesterase (PDE4NPD) and kinetoplastid (KINDReD) targets, as well as optimisation of various classes of compounds and natural products that address mechanisms associated with protozoa virulence and pathogenicity (New Medicine for Trypanosomatidic Infections – NMTrypI). An overview of the NMTrypI consortium is described in this article.
Human African trypanosomiasis (also known as sleeping sickness) is a tropical disease found in sub-Saharan Africa that is spread by the bite of an infected tsetse fly. The tsetse fly bite results in a red sore which leads to fever, swollen lymph glands and pain in muscles and joints. Subsequent to this, the nervous system can be affected, causing a variety of speech- and movement-related problems that can eventually be fatal if not treated.1 Although a number of anti-trypanosomatidic compounds have been approved for use and a pipeline of compounds in preclinical and clinical development exist, many of these are associated with undesirable characteristics such as lengthy treatment regimen, intravenous route of administration, and toxicity.1 Therefore, new anti-trypanosomatid drugs are urgently needed and this specific issue has been addressed by the NMTrypI consortium.2
Objectives of the NMTrypI consortium
The NMTrypI consortium made use of a multi-national inter-disciplinary approach to optimise multiple compound classes (pteridine, benzothiazole, miltefosine derivatives and natural products) that exhibited anti-trypanosomatid behaviour.3 Overall, the consortium was composed of SMEs, European universities, research institutes and relevant stakeholders in Africa and Brazil. The experimental approaches included optimisation of the various classes of compounds, fragment-based drug design, target and phenotypic screening, dual-target inhibition and evaluation of combination therapies.
An additional component was to use relevant pre-clinical biomarkers and proteomic profiling of compounds in order to determine their mechanism of action and the underlying reason for their efficacy. The most promising compounds were identified and evaluated in mouse, hamster and dog disease models. The project led to the discovery of multiple compound series that were progressed in the drug discovery value chain towards the lead and candidate milestones and some of these are detailed below.
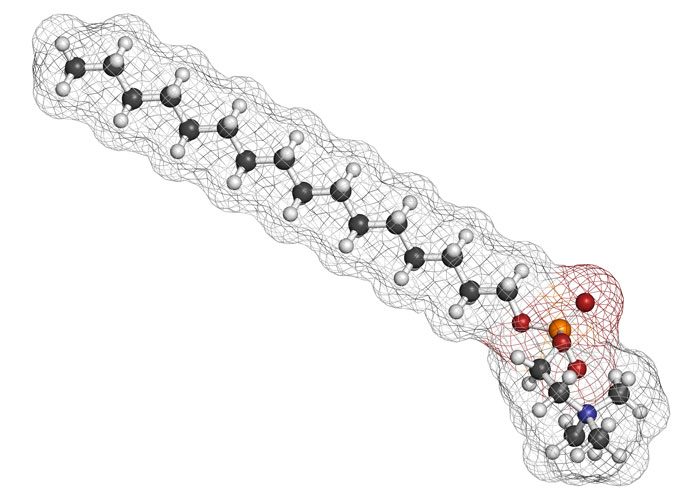

A molecule of miltefosine, which is used to treat leishmaniasis. The NMTrypI consortium investigated optimising miltefosine derivatives
Thiadiazole compounds
Pteridine reductase-1 (PTR1) is a drug target for the treatment of trypanosomiasis.4 The thiadiazole class of inhibitors of Trypanosoma brucei (Tb) PTR1 have been optimised guided by crystal structures of TbPTR1-inhibitor complexes to design new thiadiazole derivatives. The new compounds were active in appropriate target- and cell-based assays and associated with low toxicity. These findings confirmed the view that development of thiadiazoles is a promising approach for the development of anti-trypanosomatid agents.5
Flavonoid compounds
This class of compound are also inhibitors of PTR1. Although some of these are effective in vitro, they lack discernible in vivo activity due to their low bio-availability. In order to overcome these issues, a new class of flavonol-like compounds with improved potency and selectivity toward TbPTR1 were designed with input from x-ray crystallography and docking studies. Although an improvement in bioavailability was not observed subsequent to cyclodextrin complexation, this did result in reduced in vitro toxicity and increased plasma levels and therefore this provides an avenue for further optimisation.6
Crassiflorone natural product derivatives
Crassiflorone is a natural product that is a dual Tb glyceraldehyde-3-phosphate dehydrogenase (TbGAPDH)/T cruzi trypanothione reductase (TcTR) inhibitor. A small library of crassiflorone derivatives were designed and investigated for their potential as anti-trypanosomatidic agents in enzyme and L infantum, T brucei and T cruzi whole-cell parasite assays. When considering these activities in conjunction with the in vitro toxicity assays, a number of compounds that exhibited dual enzyme inhibition (TbGAPDH and TcTR) as well as inhibiting growth of the Tb bloodstream-form were identified. Although some issues with regards to compound toxicity were observed for cytochrome P450, this liability was overcome, demonstrating that this class of natural product-derived compounds can be further progressed.7
Chalcone
The chalcones are aromatic ketones that display a broad spectrum of pharmacological activities. A series of 2′-hydroxy methoxylated chalcones were synthesized and evaluated against T brucei, T cruzi and L infantum, with the most potent and selective compounds showing anti-parasitic and acceptable toxicity profiles. Subsequent pharmacokinetic studies and formulation with cyclodextrins led to an increase in oral bioavailability and acceptable half-life. Thus, further optimisation of this class of compound and improved drug delivery systems would be expected to enable the full exploitation of the potential of methoxylated 2′-hydroxychalcones.8
Summary
Due to the detrimental worldwide burden of NTD, there is a clear necessity to discover new targets and new drugs to treat such diseases. The multidisciplinary NMTrypI consortium that made use of in-vitro, in-silico and in-vivo approaches led to a number of different compound classes being designed which yielded acceptable inhibition profiles against specific targets, acceptable liability profiles and activity in cell-based parasite assays. Thus, significant chemical matter has been identified to feed the NTD drug discovery pipeline that could result in the next generation of drugs to treat these diseases.
Acknowledgment
This project has received funding from the European Union’s Seventh Framework Programme for research, technological development, and demonstration under grant agreement number 603240 (NMTrypI, New Medicine for Trypanosomatidic Infections).
References
- Field MC, Horn D, Fairlamb AH, Ferguson MA, Gray DW, Read KD, De Rycker M, Torrie LS, Wyatt PG, Wyllie S, Gilbert IH. Anti-trypanosomatid drug discovery: an ongoing challenge and a continuing need. Nat Rev Microbiol. 2017;15:217-231.
- Pierce RJ, MacDougall J, Leurs R, Costi MP. The Future of Drug Development for Neglected Tropical Diseases: How the European Commission Can Continue to Make a Difference. Trends Parasitol. 2017;33:581-583.
- http://fp7-nmtrypi.eu/
- Sienkiewicz N, Ong HB, Fairlamb AH. Trypanosoma brucei pteridine reductase 1 is essential for survival in vitro and for virulence in mice. Mol Microbiol.2010;77:658-671.
- Linciano P, Dawson A, Pöhner I, Costa DM, Sá MS, Cordeiro-da-Silva A, Luciani R, Gul S, Witt G, Ellinger B, Kuzikov M, Gribbon P, Reinshagen J, Wolf M, Behrens B, Hannaert V, Michels PAM, Nerini E, Pozzi C, di Pisa F, Landi G, Santarem N, Ferrari S, Saxena P, Lazzari S, Cannazza G, Freitas-Junior LH, Moraes CB, Pascoalino BS, Alcântara LM, Bertolacini CP, Fontana V, Wittig U, Müller W, Wade RC, Hunter WN, Mangani S, Costantino L, Costi MP. Exploiting the 2-Amino-1,3,4-thiadiazole Scaff old To Inhibit Trypanosoma brucei Pteridine Reductase in Support of Early-Stage Drug Discovery. ACS Omega. 2017;2:5666-5683.
- Borsari C, Luciani R, Pozzi C, Poehner I, Henrich S, Trande M, Cordeiro-da-Silva A, Santarem N, Baptista C, Tait A, Di Pisa F, Dello Iacono L, Landi G, Gul S, Wolf M, Kuzikov M, Ellinger B, Reinshagen J, Witt G, Gribbon P, Kohler M, Keminer O, Behrens B, Costantino L, Tejera Nevado P, Bifeld E, Eick J, Clos J, Torrado J, Jiménez-Antón MD, Corral MJ, Alunda JM, Pellati F, Wade RC, Ferrari S, Mangani S, Costi MP. Profi ling of Flavonol Derivatives for the Development of Antitrypanosomatidic Drugs. J Med Chem. 2016;59: 7598-7616.
- Uliassi E, Fiorani G, Krauth-Siegel RL, Bergamini C, Fato R, Bianchini G, Carlos Menéndez J, Molina MT, López-Montero E, Falchi F, Cavalli A, Gul S, Kuzikov M, Ellinger B, Witt G, Moraes CB, Freitas-Junior LH, Borsari C, Costi MP, Bolognesi ML. Crassifl orone derivatives that inhibit Trypanosoma brucei lyceraldehyde-3-phosphate dehydrogenase (TbGAPDH) and Trypanosoma cruzi trypanothione reductase (TcTR) and display trypanocidal activity. Eur J Med Chem.2017;141:138-148.
- Borsari C, Santarem N, Torrado J, Olías AI, Corral MJ, Baptista C, Gul S, Wolf M, Kuzikov M, Ellinger B, Witt G, Gribbon P, Reinshagen J, Linciano P, Tait A, Costantino L, Freitas-Junior LH, Moraes CB, Bruno Dos Santos P, Alcântara LM, Franco CH, Bertolacini CD, Fontana V, Tejera Nevado P, Clos J, Alunda JM, Cordeiro-da-Silva A, Ferrari S, Costi MP. Methoxylated 2′-hydroxychalcones as antiparasitic hit compounds. Eur J Med Chem.2017;126:1129-1135.
Biographies






Related topics
Biomarkers, Disease Research, Drug Leads, Drug Targets, Hit-to-Lead, In Vitro, In Vivo, Proteomics, Toxicology
Related conditions
African sleeping sickness, African trypanosomiasis
Related organisations
Fraunhofer-IME SP, University of Modena and University of Modena and Reggio Emilia
Related people
Giulia Pasini, Maria Paola Costi, Sheraz Gul








