Researchers use brain organoids to identify neural abnormalities and test gene therapy tools
Posted: 4 May 2022 | Ria Kakkad (Drug Target Review) | No comments yet
Scientists used human brain organoids to reveal how a genetic mutation associated with a profound form of autism disrupts neural development, and gene therapy tools to recover the gene’s function effectively rescued neural structure and function.

Numerous neurological and neuropsychiatric diseases, including autism spectrum disorders (ASD) and schizophrenia, have been linked to transcription factor 4 (TCF4) mutations, an essential gene in brain development. Transcription factors regulate when other genes are turned on or off, so their presence, or lack thereof, can have a domino effect in the developing embryo. However, little is known about what happens to the brain when TCF4 is mutated.
Researchers at University of California San Diego School of Medicine, US focused on Pitt-Hopkins Syndrome, an ASD caused explicitly by mutations in TCF4. Children with the genetic condition have profound cognitive and motor disabilities and are typically non-verbal. In a study published in Nature Communications, scientists used human brain organoids to reveal how a genetic mutation associated with a profound form of autism disrupts neural development. The researchers also used gene therapy tools to recover the gene’s function effectively rescued neural structure and function.
Existing mouse models of Pitt-Hopkins Syndrome fail to mimic patients’ neural characteristics accurately, so the UC San Diego team created a human research model of the disorder. Using stem cell technology, they converted patients’ skin cells into stem cells, which were then developed into three-dimensional brain organoids.
The TCF4-mutated organoids were substantially smaller than normal organoids, and many of the cells were not neurons but neural progenitors. These simple cells are meant to multiply and then mature into specialised brain cells, but some part of this process had gone awry in the mutated organoids.
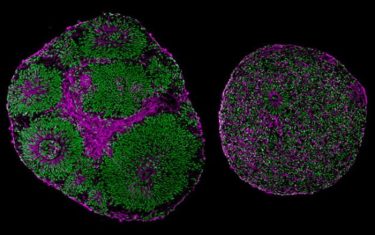

Microscopy images reveal significant differences in size and structure between brain organoids derived from a patient with Pitt-Hopkins Syndrome (right) and from a control (left)
[Credit: UC San Diego Health Sciences].
A series of experiments revealed that the TCF4 mutation led to downstream dysregulation of SOX genes and the Wnt pathway, two necessary molecular signals that guide embryonic cells to multiply, mature into neurons and migrate to the correct location in the brain.
Due to this dysregulation, neural progenitors did not multiply efficiently, and thus fewer cortical neurons were produced. Furthermore, the cells that did mature into neurons were less excitable than normal and often remained clustered together instead of arranging themselves into finely tuned neural circuits.
This atypical cellular architecture disrupted the flow of neural activity in the mutated brain organoid, which authors said would likely contribute to impaired cognitive and motor function down the line.
“We were surprised to see such major developmental issues at all these different scales, and it left us wondering what we could do to address them,” said first author Dr Fabio Papes.
The team tested two different gene therapy strategies for recovering the functional gene in brain tissue. Both methods effectively increased TCF4 levels and in doing so, corrected Pitt-Hopkins Syndrome phenotypes at molecular, cellular and electrophysiological scales.
ICYMI: Brain organoids may boost drug screening for neurological disorders
READ MORE
The researchers noted that these genetic interventions took place at a prenatal stage of brain development. In contrast, in a clinical setting, children would receive their diagnosis and treatment a few years later. Thus, clinical trials must first confirm whether a later intervention is still safe and effective. The team is currently optimising their recently licensed gene therapy tools in preparation for such a trial, in which spinal injections of the genetic vector would hopefully recover TCF4 function in the brain.
Related topics
Disease Research, Gene Testing, Gene Therapy, Neurons, Neurosciences, Organoids
Related conditions
autism spectrum disorders (ASD), Pitt-Hopkins Syndrome, Schizophrenia
Related organisations
University of California San Diego School of Medicine
Related people
Dr Fabio Papes