US researchers studied the extracellular vesicles of fibrosis and find potential avenue for new treatments and therapeutics.
Extracellular vesicles (EVs), responsible for cell-to-cell communication, might be a driver of fibrosis in systemic sclerosis, according to a study, published in Arthritis and Rheumatology.
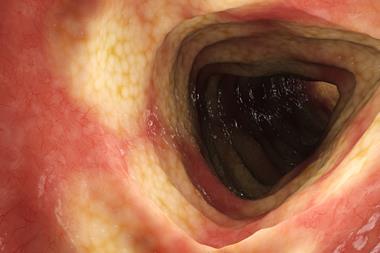
Characterised by stiff and hardening tissue known as fibrosis, systemic sclerosis (also known as scleroderma), can affect the skin as well as other organs. Most research has focused on the pathology and starting point of fibrosis, but researchers at the Medical University of South Carolina (MUSC), US, are focusing on what causes it to spread.
Their results may pave the way for therapeutics to slow the spread of fibrosis and lessen the burden of scleroderma on patients.
According to the National Institutes of Health, EVs are efficient transporters that could become a successful drug platform as they don’t illicit an immune response like synthetic versions tend to do and are widely available throughout the body.
Dr Carol Feghali-Bostwick is a Distinguished Professor in MUSC’s division of rheumatology and immunology and the SmartState and Kitty Trask Holt Endowed Chair for Scleroderma Research as well as the lead author on the paper. She points to three hallmarks of scleroderma, which is considered an autoimmune connective tissue disorder: vascular anomalies, immune system dysregulation and fibrosis. With fibrosis, cells make too much extracellular matrix components like collagen. Too many of these proteins accumulate and cause the tissues to thicken. Thick or hardened lungs for instance are unable to expand and collect enough oxygen.
Feghali-Bostwick explained that fibrosis from scleroderma as a prototypic disease in the sense that it’s very similar to fibrosis caused by other diseases. Finding ways to treat fibrosis in scleroderma patients will also treat fibrosis caused by other disorders.
“Asthma is fibrosis of the airways, alcoholic liver cirrhosis is fibrosis of the liver,” she said. “Understanding scleroderma will open the door to better understanding all these other conditions as well. And new treatment developments are likely to be effective in those other conditions.”
The researchers looked at the EVs released from the lung tissue of patients with scleroderma. It was found that not only do fibrotic lungs release more EVs than their healthy counterparts, but they release EVs with more fibrotic proteins than their healthy counterparts. Previous studies have shown correlations between EVs and the fibrotic signals they carry as cargo, and this most recent study further supports these findings.
EVs could also activate dormant fibroblasts in healthy lungs, which initiated development of fibrosis in that area and set off a chain of fibrotic spread. Feghali-Bostwick says further research is needed to determine its effect once it leaves the lungs.
EVs provide protection against cargo breakdown, which adds to their effectiveness as an intercellular communicator and supplies carrier, but it also leads to more dangerous fibrotic proliferation.
Feghali-Bostwick finds this research exciting clinically as halting EV communication or altering their cargo could become a therapeutic possibility for scleroderma patients as well as those with fibrosis due to other disorders and diseases.
“The research is still in its early stages,” she concluded. “But it’s very promising that we may be able to leverage EVs for treatment.”