Stem cells in COPD patient lungs revealed as drug target for condition
Posted: 16 April 2020 | Victoria Rees (Drug Target Review) | 1 comment
There are heightened levels of abnormal stem cells in the lungs of COPD patients, presenting a drug target that researchers are screening compounds against.
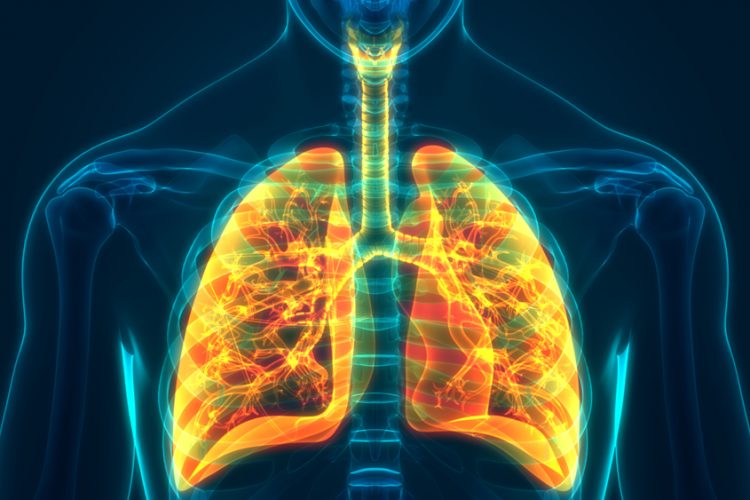

Researchers have discovered that there is an abundance of abnormal stem cells in the lungs of patients who suffer from Chronic Obstructive Pulmonary Disease (COPD). According to the researchers, these cells could the be target of novel therapeutics.
From the University of Houston, US, the researchers used single cell cloning of lung stem cells to make their discovery. The stem cells were gathered from lung fluid while performing bronchoscopies.
“We actually found that three variant cells in all COPD patients drive all the key features of the disease. One produces tremendous amounts of mucins which block the small airways, while the other two drive fibrosis and inflammation which together degrade the function of the lung. These patients have normal stem cells, though not many of them, but they are dominated by the three variant cells that together make up the disease,” said Wa Xian, research associate professor at the Stem Cell Center of the university.
Over the past decade, the researchers have developed a technology for cloning stem cells of the lungs and airways. They note that different parts of the airways yield different stem cells, related but distinguishable.
“It’s quite remarkable,” said Frank McKeon, professor of biology and biochemistry and director of the Stem Cell Center. “In the deep lung, the distal airway stem cells gave rise to both the distal tubes and the alveoli and our research indicates those are the stem cells that make it possible for lungs to regenerate on their own.”
The researchers found that, in contrast to normal lungs, COPD lungs were inundated by three unusual variant lung stem cells that are committed to form metaplastic lesions known to inhabit COPD lungs, but seen by many as a secondary effect without a causal link to the pathology of COPD. After the team’s postdoctoral fellow, Wei Rao, transplanted each of the COPD clones into immunodeficient subjects, the team found they not only gave rise to the distinct metaplastic lesions of COPD, but they separately triggered the triad of pathologies of COPD including mucus hypersecretion, fibrosis and chronic inflammation.
“The long-overlooked metaplastic lesions in COPD were, in fact, driving the disease rather than merely secondary consequences of the condition,” said McKeon.
Now that the team knows the identity of the cells that cause inflammation, fibrosis and small airway obstruction, they are screening them against libraries of drug-like molecules to discover new therapeutics.
“As we now know the specific cells responsible for COPD pathology, we can target them, much as we would cancer, with specific drugs that selectively kill them off and leave the normal cells to regenerate normal lung tissue,” said Xian.
The results can be found in Cell.
Related topics
Disease Research, Drug Targets, Research & Development, Screening, Stem Cells, Targets
Related conditions
Chronic obstructive pulmonary disease (COPD)
Related organisations
University of Houston
Related people
Frank McKeon, Wa Xian, Wei Rao







It would be great if this information and any follow-up trials were published by COPD Foundation.