Personalised organoid models for rare spinal cancer
Posted: 25 April 2022 | Ria Kakkad (Drug Target Review) | No comments yet
Scientists have successfully created viable organoids from tumour samples from five patients with a rare bone cancer called a chordoma, which has few therapeutic options.
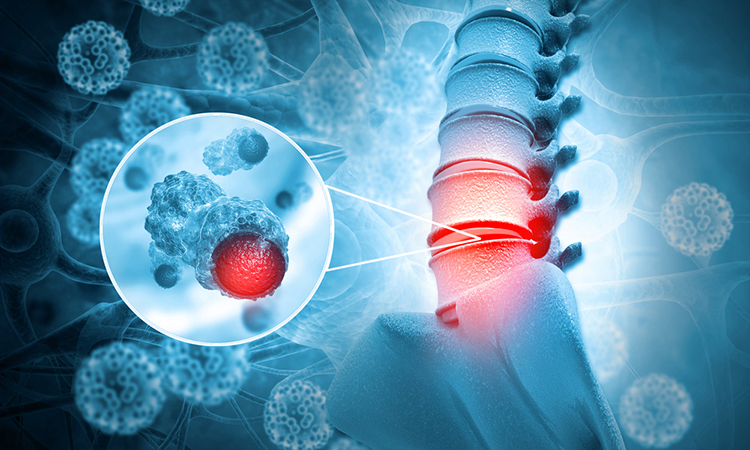
In a study led by University of California Los Angeles (UCLA), US, researchers have successfully created viable organoids from tumour samples from five patients with a rare spinal cancer, chordoma, which has few therapeutic options. The research was recently published in Science Advances.
As reported in the new study, investigators successfully created viable organoids from all samples. The patient-derived organoids showed morphologies and characteristics closely matching the actual chordoma tumours they were derived from, such as expressing a protein called Ki-67, associated with cell proliferation, and brachyury, a protein that is a well- established marker of chordoma.
The investigators then used the organoids to perform high-throughput drug screening, an automated drug discovery process that allows for large numbers of potential therapeutics to be tested at once, rather than one at a time, significantly accelerating the development and testing of potential targets and drugs. This type of large-scale screening has been key to drug development and testing, but this is its first application to patient-derived chordoma organoids.
“We have shown that the patient-derived tumour organoids we develop can be effectively screened against hundreds of drugs using our platform, which now includes machine learning approaches to study organoids growth patterns and pathway analysis to find targetable biological processes,” stated Dr Alice Soragni, study lead.
From the screening, the authors identified several drug targets and biological pathways that could be potentially pursued for therapy for chordoma. They also pinpoint the importance of a personalised approach, given the diverse responses seen among patients as well as between different tumours collected from the same patient.
ICYMI: Scientists have opened a path towards triple-negative breast cancer treatment, by creating organoids from tumour samples.
READ MORE
“Our automation-compatible approach to grow and screen patient-derived tumour organoids works well for rare carcinomas and now even slow growing bone tumours. Our work continues to be focused on generating individualised models for rare tumours, which often lack therapeutic options, with a long-term goal to leverage these results in clinic,” concluded Dr Soragni.
Related topics
Disease Research, Drug Discovery Processes, Oncology, Organoids, Screening
Related conditions
chordoma
Related organisations
University of California Los Angeles (UCLA)
Related people
Dr Alice Soragni